Just In
- 1 hr ago

- 5 hrs ago

- 6 hrs ago

- 11 hrs ago

Don't Miss
- Movies
 LSD2 Box Office Collection Day 1 Prediction: Dibakar Banerjee’s Film To Have Slow Start; Will Fail To Touch 5C
LSD2 Box Office Collection Day 1 Prediction: Dibakar Banerjee’s Film To Have Slow Start; Will Fail To Touch 5C - Finance
 1:3 Bonus Share, Rs 13.25/Share Dividend: Buy Maharatna PSU, TP Rs 355, Fundraise Approved
1:3 Bonus Share, Rs 13.25/Share Dividend: Buy Maharatna PSU, TP Rs 355, Fundraise Approved - Sports
 Michail Antonio felt officials were against West Ham after European exit
Michail Antonio felt officials were against West Ham after European exit - News
 12 Jurors Picked For Donald Trump’s Hush Money Trial, Alternate Selection Continues
12 Jurors Picked For Donald Trump’s Hush Money Trial, Alternate Selection Continues - Automobiles
 Aprilia RS 457 Accessories: A Detailed Look At The Prices
Aprilia RS 457 Accessories: A Detailed Look At The Prices - Education
 Karnataka SSLC Result 2024 Soon, Know How to Check Through Website, SMS and Digilocker
Karnataka SSLC Result 2024 Soon, Know How to Check Through Website, SMS and Digilocker - Technology
 Nothing Ear, Ear a With ANC, Up to 42.5 Hours of Battery Launched; Check Price and Availability
Nothing Ear, Ear a With ANC, Up to 42.5 Hours of Battery Launched; Check Price and Availability - Travel
Telangana's Waterfall: A Serene Escape Into Nature's Marvels
Psoriasis: Types, Causes, Symptoms, Risk Factors, Diagnosis And Treatment
Psoriasis is a chronic, inflammatory autoimmune skin condition that causes red, itchy scaly patches on the skin, which usually tend to affect the elbows, knees, scalp, lower back, soles of the feet and palms of the hands. It is estimated that between 0.5 per cent to 1 per cent of children and 2 per cent to 3 per cent of people worldwide are affected by psoriasis [1].
Psoriasis may occur in people aged between 20 to 30 years or later in life between 50 to 60 years [1].

What Causes Psoriasis? [2]
The exact cause of psoriasis is not known, however, a combination of many elements including genetics and environmental factors in combination with dysfunction of the immune system and disruption of the skin barrier could play a major role in the development of psoriasis.
• Genetics - Children have a 20 per cent chance of having psoriasis if their one parent has it and if both parents have it children have a 65 per cent chance of getting psoriasis. The mutation of two genes IL36RN and CARD14 have been found to cause psoriasis by affecting both the skin and immune system.
• Environmental factors - Several environmental factors can cause psoriasis. These include physical trauma, drug reactions, infections, stress, obesity, alcohol and smoking.

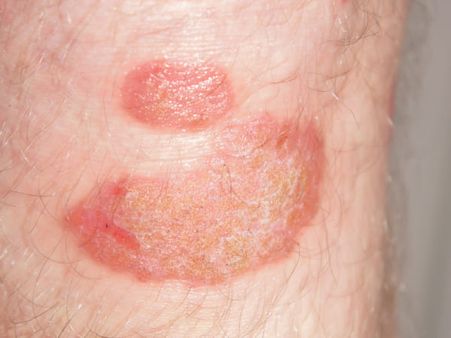
Types Of Psoriasis
1. Plaque psoriasis -Plaque psoriasis also known as Psoriasis vulgaris is the most common type of psoriasis which affects approximately 85 per cent to 90 per cent of psoriatic patients. This type of psoriasis is characterised by raised areas of red inflamed skin covered with silvery-white scaly skin. These areas are also known as plaques and are mainly seen on the elbows, knees, scalp and back[1].
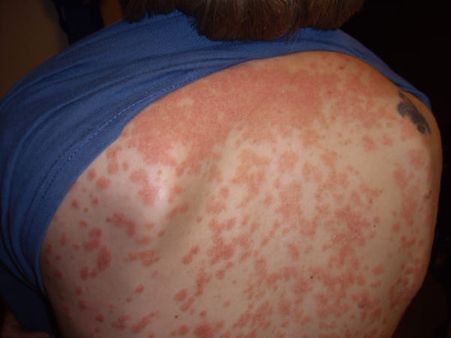
2. Guttate psoriasis -This type of psoriasis is usually common in childhood or young adulthood. It is characterised by multiple small scaly, red plaques on the limbs and trunk. It is often triggered by streptococcal infection[1].
3. Pustular psoriasis - It is more common in adults. Pustular psoriasis is characterised by small, white pus-filled blisters which are surrounded by red, inflamed skin. They usually develop in certain areas of the body like the hands and feet [3].
4. Inverse psoriasis - Inverse psoriasis is a rare type of psoriasis that affects three to seven per cent of psoriasis patients [4]. It is characterised by red, shiny, inflamed skin that develops in the underarms, navel, groin and buttocks.
5. Erythrodermic psoriasis -It is the least common type of psoriasis but it is the most severe form of psoriasis. Red lesions often cover large areas of the body involving nearly around 90 per cent of body surface area and may cause severe dryness, itching, swelling and pain. This form of psoriasis can be fatal as the inflammation and exfoliation disrupt the body's thermoregulation[5].


Symptoms Of Psoriasis
The symptoms of psoriasis vary depending on the type you have. However, the common symptoms are:
•
Red,
flaky
patches
of
skin
covered
with
thick
silver-coloured
scales
•
Dry,
cracked
skin
that
can
itch
or
bleed
•
Red,
flaky
patches
of
skin
causing
intense
itching
or
burning
sensation.
•
Thick,
pitted
nails
•
Painful,
swollen
joints
According to the National Psoriasis Foundation, the symptoms of psoriasis may range from mild to severe. Mild psoriasis covers less than 3 per cent of the body, moderate psoriasis covers between 3 to 10 per cent of the body and severe psoriasis covers more than 10 per cent of the body [6].

Risk Factors Of Psoriasis
•
Family
history
[7]
•
Stress
•
Consumption
of
alcohol
•
Smoking


Complications Of Psoriasis
•
Psoriatic
arthritis
[8]
•
Obesity
•
Eye
conditions
such
as
blepharitis
and
uveitis
[9]
•
Heart
disease
[10]
•
Type
2
diabetes
[11]
•
High
blood
pressure
[12]
•
Autoimmune
diseases
like
sclerosis,
celiac
disease
and
Crohn's
disease.
Diagnosis Of Psoriasis
According to the National Psoriasis Foundation, there are no blood tests to diagnose psoriasis. A dermatologist will ask about your family history and examine the affected skin and may take a piece of the skin and carry out a skin biopsy. This will help rule out psoriasis or any other skin condition.
Treatment Of Psoriasis
Topical treatments [1]
Mild psoriasis is treated with topical therapies which include the following:
• Coal tar - Studies have shown that coal tar has been used for treating psoriasis due to its anti-proliferative activity. However, side effects of coal tar has been shown in psoriasis patients which include poor tolerance due to its odour and staining, skin irritation, contact dermatitis, photosensitivity and folliculitis.
• Dithranol (anthralin) - It is an anthracycline that has been used for treating psoriasis. This form of treatment is not being used much because of more cosmetically acceptable therapies. The side effects of dithranol include skin irritation and skin discolouration and when used in excess it causes blistering and necrosis.
• Vitamin D analogs - It is used for treating mild to moderate psoriasis. Currently, the vitamin D analogs for treating psoriasis are calcitriol, tacalcitol, and calcipotriol, however, vitamin D analogs causes common side effects such as skin irritation and photosensitivity.
Globally, between 30 to 50 per cent of psoriasis patients showed a marked improvement or completely recovered after four to six weeks of using vitamin D analogs.
• Corticosteroids - It is the most frequently used topical medication for psoriasis and used for all grades of plaque psoriasis. The effectiveness and side effects of corticosteroids depend on the potency, vehicle, occlusion and patient compliance.
• Keratolytics - The keratolytics agents such as salicylic acid, urea, glycolic acid and propylene glycol are used for the treatment of psoriasis.
• Calcineurin inhibitors - Calcineurin inhibitors like tacrolimus and pimecrolimus have been used off-label to treat facial lesions and lesions which appear in skin folds.
• Retinoids - A topical retinoid called tazarotene is used for the treatment of psoriasis. Oral retinoids, when used in combination with UV light treatment, has been shown to be more effective in patients with plaque psoriasis.
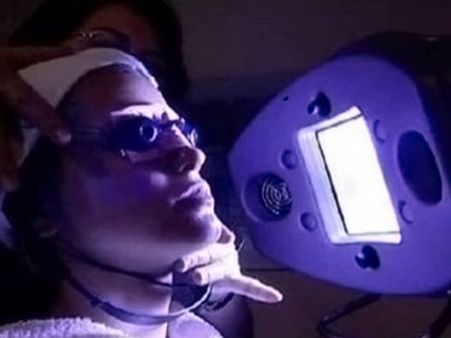
Phototherapy [1]
Phototherapy is commonly used for the treatment of moderate to severe psoriasis. This treatment involves exposing the skin to ultraviolet light, which will help slow down cell growth, lower irritation and suppress immune activity.
UVA light is considered more effective than UVB light for the treatment of psoriasis, but it's considered more carcinogenic and causes photoaging.
Systemic therapies [1]
Systemic therapies are used for the treatment of moderate to severe psoriasis and psoriatic arthritis. Systemic therapies include biologic treatment, methotrexate and cyclosporine.

Tips For Living Well With Psoriasis
•
Maintain
a
healthy
weight
•
Eat
a
well-balanced
diet
•
Do
not
smoke
or
drink
alcohol
•
Reduce
stress
by
practising
yoga,
meditation
and
exercise
Common FAQs
Q. What does psoriasis look like?'
A. Psoriasis appears as red, thick, itchy, scaly patches on the skin that can be small or large.
Q. How do I know if it's eczema or psoriasis?
A. In the early stages, eczema and psoriasis may look similar because the way they appear, as a red, itchy inflamed skin. Overtime, the disease will spread in certain areas of the body which will make it easier to differentiate. Psoriasis will show up on the scalp, face, skin folds, genitals, hands, feet and nails. And eczema will develop on the face, wrists, hands, feet or back of the knees. However, it is important to show a dermatologist immediately if you notice red, itchy skin.
Q. What happens if you don't treat psoriasis?
A. If you don't treat psoriasis it can lead to serious medical complications.
Q. What is the best home remedy for psoriasis?
A. Salt baths, aloe vera, turmeric, omega 3 fatty acids, Oregon grape are some home remedies for psoriasis.
Q. Is psoriasis contagious?
A. No, a person can't get the disease from someone else and can't pass it to someone else through skin-to-skin contact. You can't contract the disease by touching someone who has psoriasis.

-
 wellnessCan Drinking Milk After Eating Fish Cause Skin Diseases?
wellnessCan Drinking Milk After Eating Fish Cause Skin Diseases? -
 skin care7 Beauty Tips For People With Psoriasis
skin care7 Beauty Tips For People With Psoriasis -
 wellness10 Natural Treatments And Home Remedies For Psoriasis Relief
wellness10 Natural Treatments And Home Remedies For Psoriasis Relief -
 wellnessBiologics: What Are They & How They Help Treat Psoriasis
wellnessBiologics: What Are They & How They Help Treat Psoriasis -
 disorders curePenile Allergy: Causes, Home Remedies And Prevention
disorders curePenile Allergy: Causes, Home Remedies And Prevention -
 disorders cureSebopsoriasis: Causes, Symptoms, Diagnosis And Treatment
disorders cureSebopsoriasis: Causes, Symptoms, Diagnosis And Treatment -
 wellnessCan Psoriasis Affect Your Eyes?
wellnessCan Psoriasis Affect Your Eyes? -
 wellness10 Reasons Your Butt Itches Like Crazy All the Time
wellness10 Reasons Your Butt Itches Like Crazy All the Time -
 wellnessSkin Conditions That Actually Signal Other Health Problems
wellnessSkin Conditions That Actually Signal Other Health Problems -
 nutritionFoods That Trigger Psoriasis
nutritionFoods That Trigger Psoriasis -
 disorders cureNeem Oil Can Cure Psoriasis
disorders cureNeem Oil Can Cure Psoriasis -
 disorders cureBeer Can Get You Psoriasis
disorders cureBeer Can Get You Psoriasis


 Click it and Unblock the Notifications
Click it and Unblock the Notifications



