Latest Updates
-
 The Perfect Without Eggs Trick: Eggless Cake Recipe
The Perfect Without Eggs Trick: Eggless Cake Recipe -
 Horoscope for Today April 22, 2026 - Practical Steps for Steady Progress
Horoscope for Today April 22, 2026 - Practical Steps for Steady Progress -
 Dipika Kakar Faces New Health Concern After Cancer Surgery: Two Cysts Detected In MRI, Immunotherapy Begins
Dipika Kakar Faces New Health Concern After Cancer Surgery: Two Cysts Detected In MRI, Immunotherapy Begins -
 Anthony Anderson Interview On Mentorship, Giving Back, And Uplifting The Next Generation
Anthony Anderson Interview On Mentorship, Giving Back, And Uplifting The Next Generation -
 Rich Creamy Dinner Special Paneer Masala Recipe
Rich Creamy Dinner Special Paneer Masala Recipe -
 Autism Awareness Month 2026: Why School Holidays Feel Overwhelming For Autistic Children And What Helps
Autism Awareness Month 2026: Why School Holidays Feel Overwhelming For Autistic Children And What Helps -
 Try The Viral Dhurandhar Aalam Doodh Soda This Summer, Plus A Healthier Twist To Stay Cool And Refreshed
Try The Viral Dhurandhar Aalam Doodh Soda This Summer, Plus A Healthier Twist To Stay Cool And Refreshed -
 The Ultimate Soft Banana Cake Recipe
The Ultimate Soft Banana Cake Recipe -
 7.7 Magnitude Quake Strikes Sanriku Coast, Megaquake Advisory Issued: Inside Japan’s Rapid Alert System
7.7 Magnitude Quake Strikes Sanriku Coast, Megaquake Advisory Issued: Inside Japan’s Rapid Alert System -
 Aishwarya Rai Marks 19 Years With Abhishek Bachchan In Anniversary Post, From Co-Stars To Marriage
Aishwarya Rai Marks 19 Years With Abhishek Bachchan In Anniversary Post, From Co-Stars To Marriage
Facts Behind Jaundice In Newborns
Jaundice is one of the commonest reasons parents visit Paediatricians. It refers to the yellow colouration of the skin and the white of the eye (sclera) caused by the accumulation of a yellow pigment called "bilirubin" in the skin and mucus membranes. It is normal for everyone to have low levels of bilirubin in their blood.
Jaundice has many causes and we are sure everyone will know liver infection like hepatitis causes jaundice. But babies are peculiar in that so they get jaundice for various normal reasons - hence it is called PHYSIOLOGICAL jaundice.

Approximately 60 percent of full-term and 80 percent of premature babies develop jaundice in the first week of life, and in most of the babies with jaundice there is no underlying disease, and this early jaundice (termed 'physiological jaundice') is generally harmless. The condition is more common in babies because:
Babies make more bilirubin than adults do since they have more turnover of blood cells.
A newborn baby's still developing liver may not yet be able to remove adequate bilirubin from the blood.
Too large an amount of bilirubin is reabsorbed from the intestines before the baby gets rid of it in the stool.

HOW IS JAUNDICE CAUSED IN NEWBORN BABIES?
The yellow colouring in the skin is caused by a build up of a pigment called bilirubin - a naturally occurring product from the break down of red blood cells. These cells have a life span of about 120 days in an adult and about 80 to 100 days in newborn babies.
The body is constantly producing new blood cells as old ones dies.In the uterus the foetus has a higher level of red blood cells to transport oxygen around the body.
After delivery use of the lungs results in the baby not needing as many red blood cells to adequately oxygenate the body. As red blood cells break down, they form bilirubin initially in a fat soluble or an unconjugated form.
This cannot be excreted in the bile to the gut, or by the kidneys into the urine.
Hence, bilirubin is transported to the liver to be "processed or conjugated" into a water-soluble form and excreted into the bile and urine.
If the red blood cells breaks down faster than the immature liver in the newborn babies can cope with processing then the bilirubin will accumulate. Having an affinity for fatty tissue the yellow colouring will be noticed in the skin and the white of the eyes.
CAUSES OF JAUNDICE
There are many causes and contributing factors to jaundice, but the most common cause is physiological and will generally require no treatment and resolve in about 1 to 2 weeks.
Some of the more common factors that may contribute to jaundice in newborn babies include:
- Prematurity
- Low birth weight
- Trauma associated with delivery if baby is bruised.
- Cephalhaematoma (a swelling over a section of the skull that feels very soft to touch) and may take several days to go down.
- Blood group maternal- infant incompatibility ex: some mothers may be O negative and babies may be B+ve - these sort of combinations cause jaundice to appear much more quickly than 2 days after birth (see below)
- Rhesus Disease- This occurs if mother has a negative blood group and baby has a positive blood group. If mother becomes sensitised and produces antibodies - these can cross to baby via the placenta and will result in faster breakdown of baby's blood increasing jaundice.
- This is not very common as mothers with negative blood groups are now given Anti-D injection following delivery if required. This protects subsequent pregnancies from jaundice occurring from Rhesus Disease.
- Delay in passage of meconium (babies first "blackish-greenish stools). High levels of bilirubin in meconium some of which is re-absorbed raising bilirubin levels.
Infection
Infant of a diabetic mother i.e., if a mother has diabetes during pregnancy
High red cell count- In utero, a higher red cell count is required for transportation of oxygen to the body.

History & Examination- Features Particularly Relevant To Jaundice
Visual assessment of bilirubin level is unreliable:
- Is the infant unwell? (sepsis & GIT obstruction can cause jaundice)
- Is there dehydration or poor weight gain? (both exacerbate jaundice)
- Jaundice before 48 hrs of age (suggests haemolysis)
- Onset of jaundice after 3 days of age (more likely to be pathological)
- Birth trauma such as cephalhaematoma, significant bruising (breakdown of heme)
- Maternal history (blood group, viral serology)
- Family history of haemolytic disease (ABO/G6PD, spherocytosis)
- Dark urine or pale stools (suggest biliary obstruction)
- Level of icterus in terms of cephalocaudal progression (but often unreliable)
- Plethora (may suggest polycythaemia)
- Hepatosplenomegaly (viral hepatitis, metabolic problems)
TREATMENT OF JAUNDICE
Sometimes, your pediatrician may order a blood test to assess the level of jaundice. Though we call it Physiological, sometimes if the level of jaundice is high because of fat solubility it can cross to the brain (via blood-brain barrier) and cause brain damage called KERNICTERUS.
This condition is rare in modern days because of better awareness but if it does happen then can cause deafness, brain damage and eye problems. So to prevent this - the level of jaundice is sometimes 'assessed' to see whether the baby needs treatment.
In many cases no treatment is required and will resolve in 1-2 weeks. Ensuring that the baby feeds early and regularly - the baby will pass more stools and hence will stimulate the intestine so that the bilirubin is excreted in stools and its re-absorption in the intestines is minimised.
But 3 to 4 percent of babies may require treatment to reduce the levels. One way to reduce the level of jaundice is to expose baby's skin to light, a process called PHOTOTHERAPY (Light Treatment).
PHOTOTHERAPY
Phototherapy is the use of white and blue fluorescent lights. The lights change the bilirubin into a more water-soluble form, so that the kidneys can get rid of it rather than the liver, which can be immature in newborn babies.
Baby's eyes are covered to protect them from the bright light.
Baby may have skin rashes or loose, greenish bowel movements. This is temporary and should stop when the phototherapy is discontinued. Phototherapy is safe, but is used only when needed.
Most parents know that the sunlight helps - indeed that's how phototherapy came into existence, because in Europe they used to see more jaundiced babies in winter than summer when they realised sunlight had something to do!
But we don't recommend babies being put in sunlight directly - purely because the wave length of the Ultraviolet rays what we require to treat the baby is "controlled" with phototherapy equipment whereas the natural sunlight may have harmful rays for the immature newborn skin.
In most of the hospitals, once a baby requires treatment with phototherapy - baby will be separated from the mother and taken to Neonatal Unit where the treatment will be administered.
This causes separation of the mother & baby and an emotional trauma for the mother and feeding difficulties for the mother who may be shy to breast feed in the nursery in front of the other staff.
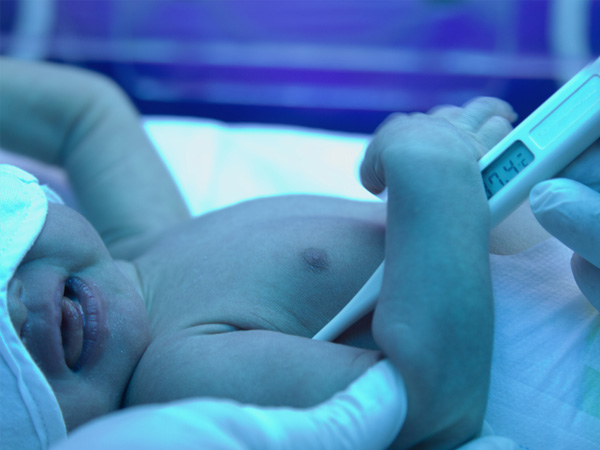
At Cloudnine we are using a new equipment called "Billi Blanket" or LED. Now with the advanced technology we have LED or "billiblanket" through which babies can be cuddled, kissed and breastfed when receiving phototherapy!
Once the level of jaundice comes down to acceptable levels, phototherapy is stopped and baby is back to 'normal'.
Billi Blanket & LED treatment has other advantages too.
- It is revolutionary - Since the treatment can be administered in the same room as the mother and there is no separation of the baby and the mother.
- There is no problem for the babies either -There in no need to "cover their eyes" from the bright light of conventional phototherapy which upsets most of the parents.
- Breastfeeding is already a difficult process for most of the new mothers. But now it can happen at the comfort of their own room rather than in the neonatal unit.
- Babies can "receive phototherapy" still while being cuddled and fed.
- This being COLD light, reduces potential for insensible water loss.
But some babies get a different type of jaundice called, Breastmilk jaundice usually after 1 to 2 weeks and this is not a reason to stop breastfeeding and does not require treatment.
Discharge instructions
- Recheck bilirubin in 24-48 hours if it at borderline level or still rising
- Parents should be advised to represent if:
- Stools become pale or urine becomes dark
- Baby is unwell or feeding poorly
- Jaundice prolonged beyond 2 weeks, for term or 3 weeks, for pre-term babies.



 Click it and Unblock the Notifications
Click it and Unblock the Notifications
