Latest Updates
-
 Crispy Corn Recipe: The Crunchy Snack Everyone Loves!
Crispy Corn Recipe: The Crunchy Snack Everyone Loves! -
 Asha Bhosle Children And Grandchildren: Where Are They Now? Full Details Inside
Asha Bhosle Children And Grandchildren: Where Are They Now? Full Details Inside -
 Asha Bhosle Passes Away At 92, Funeral On Monday: From Overlooked Beginnings To A Legendary Musical Journey
Asha Bhosle Passes Away At 92, Funeral On Monday: From Overlooked Beginnings To A Legendary Musical Journey -
 Vishu 2026: April 14th Or 15th? Significance And History Of The Malayalam New Year Festival
Vishu 2026: April 14th Or 15th? Significance And History Of The Malayalam New Year Festival -
 Masoor Dal Recipe: Your Simple Protein Rich Meal Solution
Masoor Dal Recipe: Your Simple Protein Rich Meal Solution -
 Asha Bhosle Hospitalised With Chest Infection: What Exhaustion In The Elderly Can Indicate About Health
Asha Bhosle Hospitalised With Chest Infection: What Exhaustion In The Elderly Can Indicate About Health -
 Your Ultimate Detox Morning Drink: The Perfect Lemon Tea Recipe
Your Ultimate Detox Morning Drink: The Perfect Lemon Tea Recipe -
 Horoscope for Today April 12, 2026 - Small Choices Create Steady Wins
Horoscope for Today April 12, 2026 - Small Choices Create Steady Wins -
 Makeup Hacks 101: 6 Bollywood Celebrity Makeup Hacks That Make You Look Camera Ready
Makeup Hacks 101: 6 Bollywood Celebrity Makeup Hacks That Make You Look Camera Ready -
 Your Light Comfort Healing Bowl Chicken Soup Recipe
Your Light Comfort Healing Bowl Chicken Soup Recipe
What Is Typhus? Causes, Symptoms, Treatment And Prevention
Typhus has been in existence since the very early of times. It has been acknowledged as one of the most devastating diseases throughout history, especially during the wartimes. The outbreak of typhus was initially recorded in 1489, during the Spanish army siege of Granada. It was during the early 20th century, Charles Nicolle, a French bacteriologist noticed the possible impact of a hot water shower on the typhus affected population.
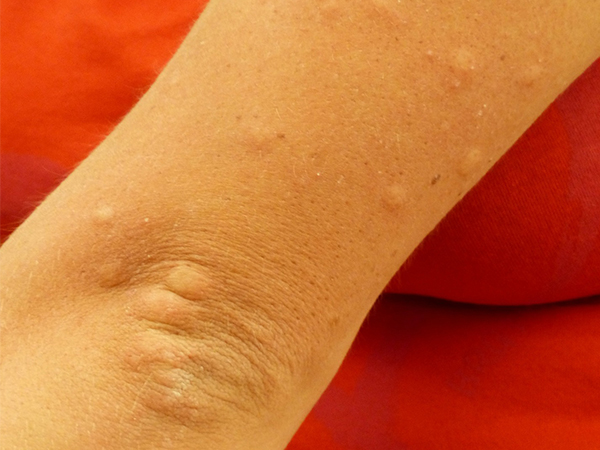
Currently, typhus is recorded in specific parts of the world, such as Eastern Africa, Asia, and certain areas in Central and South America. Even to this day, there have been no known vaccines [2] available for the prevention and cure of typhus other than improved hygienic practices, use of antibiotics and effective insecticides. But, studies have revealed a prominent contraction in the occurrence of typhus in the current times.
What Is Typhus?
Typhus is a bacterial disease caused by Rickettsia bacteria. The bacterial disease or infection is spread by fleas, lice or mites. Also known as typhus fever, typhus is a cluster of infectious[1] diseases which include, epidemic typhus, murine typhus, and scrub typhus.
The infection is spread through the arthropods, that is, invertebrate animals such as mites, lice, or ticks transmit the bacteria through biting. The insect bite can leave a mark on the body, which can further open the skin if scratched. Once the bacteria come in contact with the open skin, it will gain access to the bloodstream; continuing to reproduce and grow.
How Do You Contract Typhus?
Usually, you can catch typhus in the event of an insect bite. It is not transmitted from one person to the other like flu or the common cold. Infected lice, fleas or mites that are found on small animals such as rats, squirrels, and cats are the vehicles of the bacterial infection.
In addition to that, the insects become the carriers of the infection when it feeds on the blood of an infected rodent or an infected person. One of the most common ways through which you can contract typhus is by coming in contact with bed sheets infested with the bacterium carrying arthropods.
Likewise, the infection can spread through the excreta of the arthropods. If you scratch the bitten area where the mice or lice have been feeding on, the bacteria in the excreta will enter the bloodstream through the minute wounds contrived through scratching.
The chances of incurring typhus are high in overcrowded places such as travel hostels, places with a lot of bushes, [3] and unhygienic public washrooms.
Types & Causes Of Typhus
There are three different types of typhus. Each type of typhus is caused by a specific type of bacterium, and are suffused through different types of arthropods.
- Epidemic (louse-borne) typhus is caused by the Rickettsia prowazekii bacterium and the body louse is the carrier of this infection. It can also be transmitted through ticks. The micro abrasions present in your skin acts as the medium[4] for the pathogen-laden excreta to enter your bloodstream. The infection can be found around the globe but is generally found in areas that promote lice infestation, such as places with poor sanitation and overpopulated places. Epidemic typhus is the most severe form of typhus as it can infect a large number of population in a short period of time.
- Endemic (murine) typhus, also known as murine typhus is caused by the Rickettsia typhi bacteria. It is transmitted by the cat flea[5] or the rat flea. Murine typhus is not limited to a specific region, as it is spread across the globe. However, it is prominently found in regions with tropical and subtropical climates. It is easily contracted by people[6] who are in close contact with rats.
- Scrub typhus is caused by the Orientia tsutsugamushi bacteria. Also termed as the tsutsugamushi disease, scrub typhus is carried by trombiculid mites. Scrub typhus[7] is most commonly found in Australia, Asia, Papua New Guinea and the Pacific Islands. The carriers contrive the bacteria while feeding on the infected blood of a person (epidemic typhus) or a rodent.
You can get infected with scrub typhus in disparate ways such as sleeping on a sheet infested with mites[8] , through small openings in your skin (wounds) and also the faeces of the mites.
Symptoms Of Different Types Of Typhus
The three types of typhus have slightly variant symptoms, but there are few that are common to all the three types[9] , such as
- fever
- chills
- rash
- headache
- dry cough or hacking
- muscle and joint pain
Apart from this, each of the typhus has its own symptoms. The symptoms of epidemic typhus appear suddenly and the major symptoms[10] include
- lack of alertness, delirium, and confusion
- high fever with chills (above 102.2°F)
- severe headache
- severe joint and muscle pain
- dry cough
- sensitivity to bright light
- low blood pressure
- rashes on the chest or back, which spreads.
The symptoms of endemic typhus last between 10 to 12 days. Even though the symptoms are closely similar to that of epidemic typhus[11] , it is less severe in comparison. It includes
- back pain
- abdominal pain
- extremely high fever (105°F to 106°F), which can last up to two weeks
- dry cough and hacking
- vomiting and nausea
- muscle and joint pain
- severe headache
- dull red rashes on the middle part of the body, which spreads.
The symptoms of scrub typhus begin to show within the first ten days of being bitten. A bit more extreme than the other two types, scrub typhus can be fatal for people suffering from any sort of severe illness[12] as it can result in bleeding and organ failure. The symptoms include
- rashes
- enlarged lymph nodes
- confusion, and in some extreme cases can cause coma
- body and muscle pain
- fever and chills
- severe headache
- a dark, scab-like formation in the bitten area.
Diagnosis Of Typhus
In case you suspect the development of typhus in you, the doctor will be needing a detailed description of the symptoms and a physical examination. Providing your medical history is important as it will help the doctor to analyse your condition on an easier note.
It is preferable to inform your doctor about your living condition that is if you are residing in a crowded setting, if there are any typhus outbreaks in your locality or if you have travelled recently. The diagnosis of typhus[13] is a bit tricky and difficult as it possesses the similar symptoms as malaria, brucellosis and dengue.
The most common tests applied for the diagnosis of typhus include
- immunofluorescence test, where the doctor will use fluorescent dyes to detect the samples taken from your bloodstream to detect possible typhus antigen
- Western blot, to detect and analyse the presence of typhus
- skin biopsy, where a sample of your skin which has been affected by rashes will be tested in the lab
- blood tests, where your blood will be extracted to analyse the presence of typhus.
Treatment For Typhus
Although there is no specific treatment for typhus, antibiotics are being used currently. Sooner the application, better the effectiveness. The application varies according to the individuals affected.
- Doxycycline is the most proffered treatment. Scrub typhus must be treated with doxycycline and it can be given to people of any age. Doxycycline has been found to incur the most efficient result in a short span of time.
- Chloramphenicol is mostly used in individuals who are not pregnant or breastfeeding. It is mostly applicable for epidemic typhus.
- Ciprofloxacin[14] is issued for individuals who are unable to receive the antibiotic doxycycline.
How To Prevent Typhus
Consequently, there are no specific ways to prevent the outbreak and occurrence of typhus. Even though a vaccine for epidemic typhus was developed during the World War II, the declining number of typhus cases resulted in ceasing the manufacturing of the vaccine. As there are no specific medicines for the bacterial disease[15] , you can adopt the following measures to prevent and avoid the development of typhus.
- One of the easiest prevention methods is to avoid the breeding of pests and lice that spread the disease.
- Always maintain personal hygiene.
- Avoid travelling to overpopulated regions with low hygiene quality.
- Use insect repellents.
- In cases of extreme emergency, consume chemoprophylaxis with doxycycline as a preventive measure.
- Be careful not to use the repellents on babies[16] or children.
- Cover yourself on travelling to vegetated areas.
- Apply permethrin (kills chiggers) or purchase permethrin induced boots, camping gear etc.
Is Typhus Deadly?
Before the 20th century, there have been reports of death from typhus especially epidemic typhus. In the current era, as people are becoming increasingly aware of the need to maintain hygiene, less and less number of deaths[17] have been reported. Endemic typhus is rarely deadly, even if the affected person is not subjected to any treatment.
Disclaimer: The information provided in this article is for general informational and educational purposes only and is not intended as a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or a qualified healthcare provider with any questions you may have regarding a medical condition.
A high number of deaths have been reported amongst the older adults and malnourished people, due to the lack of a strong immune system. In the case of epidemic typhus, there has been a reported mortality rate of 10 to 60% and 30% in scrub typhus; in the event of lack of treatment. Children[18] diagnosed with typhus mostly recover. Only a reported 4% of deaths have been reported in the case of endemic typhus.
- [1] Zinsser, H. (1934). Varieties Of Typhus Virus And The Epidemiology Of The American Form Of European Typhus Fever (BRILL'S Disease.). American Journal of Epidemiology, 20(3), 513-532.
- [2] Gross, L. (1996). How Charles Nicolle of the Pasteur Institute discovered that epidemic typhus is transmitted by lice: reminiscences from my years at the Pasteur Institute in Paris. Proceedings of the National Academy of Sciences of the United States of America, 93(20), 10539.
- [3] Bechah, Y., Capo, C., Mege, J. L., & Raoult, D. (2008). Epidemic typhus. The Lancet infectious diseases, 8(7), 417-426.
- [4] Akram, S. M., & Prakash, V. (2017). Rickettsia Prowazekii (Epidemic Typhus)
- [5] Howard, A., & Fergie, J. (2018). Murine Typhus in South Texas Children: An 18-year Review. The Pediatric infectious disease journal, 37(11), 1071-1076.
- [6] Peniche Lara, G., Dzul-Rosado, K. R., Zavala Velázquez, J. E., & Zavala-Castro, J. (2012). Murine Typhus: Clinical and epidemiological aspects. Colombia Médica, 43(2), 175-180.
- [7] Typhus, S. (2010). Diagnosis and treatment of scrub typhus–the Indian scenario. JAPI, 58, 11.
- [8] Koh, G. C., Maude, R. J., Paris, D. H., Newton, P. N., & Blacksell, S. D. (2010). Diagnosis of scrub typhus. The American journal of tropical medicine and hygiene, 82(3), 368-370.
- [9] Ogawa, M., Hagiwara, T., Kishimoto, T., Shiga, S., Yoshida, Y., Furuya, Y., ... & Masukawa, K. (2002). Scrub typhus in Japan: epidemiology and clinical features of cases reported in 1998. The American journal of tropical medicine and hygiene, 67(2), 162-165.
- [10] Akram, S. M., & Prakash, V. (2017). Rickettsia Prowazekii (Epidemic Typhus).
- [11] Varghese, G. M., Janardhanan, J., Trowbridge, P., Peter, J. V., Prakash, J. A., Sathyendra, S., ... & Mathai, D. (2013). Scrub typhus in South India: clinical and laboratory manifestations, genetic variability, and outcome. International Journal of Infectious Diseases, 17(11), e981-e987.
- [12] Ramasubramanian, V., & Senthur Nambi, P. (2013). Scrub typhus. Medicine Update. India: Association of Physicians of India, 19-22.
- [13] Mazumder, R. N., Pietroni, M. A., Mosabbir, N., & Salam, M. A. (2009). Typhus fever: An overlooked diagnosis. Journal of health, population, and nutrition, 27(3), 419.
- [14] Kaore, S. N., Sharma, P., Yadav, V. K., Sharma, R., Kaore, N. M., & Langade, D. G. Treatment Update for Scrub Typhus.
- [15] Conlon, J. M. (2014). The historical impact of epidemic typhus. Dostupno na http://entomology. montana. edu/historybug/TYPHUS-Conlon. pdf, pristupljeno, 15.
- [16] Watt, G., & Parola, P. (2003). Scrub typhus and tropical rickettsioses. Current opinion in infectious diseases, 16(5), 429-436.
- [17] Snyder, J. C. (1947). Typhus fever in the second world war. California medicine, 66(1), 3.
- [18] Massung, R. F., Davis, L. E., Slater, K., McKechnie, D. B., & Puerzer, M. (2001). Epidemic typhus meningitis in the southwestern United States. Clinical infectious diseases, 32(6), 979-982.



 Click it and Unblock the Notifications
Click it and Unblock the Notifications












