Latest Updates
-
 Sita Navami 2026: Puja Muhurat, Vrat Vidhi And Spiritual Benefits For Stronger Relationships
Sita Navami 2026: Puja Muhurat, Vrat Vidhi And Spiritual Benefits For Stronger Relationships -
 World Malaria Day 2026: Date, History, Significance, and Why It Matters
World Malaria Day 2026: Date, History, Significance, and Why It Matters -
 Bakery Style Soft Texture Banana Cake Recipe
Bakery Style Soft Texture Banana Cake Recipe -
 Horoscope for Today April 25, 2026 - Steady Steps, Clear Focus, Practical Gains
Horoscope for Today April 25, 2026 - Steady Steps, Clear Focus, Practical Gains -
 Rich Mughlai Special Chicken Korma Recipe
Rich Mughlai Special Chicken Korma Recipe -
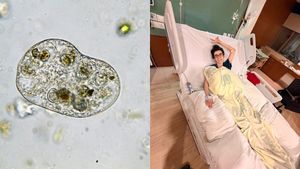 A Hidden Foodborne Infection: What You Should Know About Cyclospora
A Hidden Foodborne Infection: What You Should Know About Cyclospora -
 Melt-in-Mouth Sweet Mysore Pak Recipe: A Classic Indian Delight
Melt-in-Mouth Sweet Mysore Pak Recipe: A Classic Indian Delight -
 Between Meetings and Meals: Why American Pecans Are the Ideal Midday Snack
Between Meetings and Meals: Why American Pecans Are the Ideal Midday Snack -
 Skincare Hacks 101: 7 Summer Hacks That Actually Work in 40°C Heat
Skincare Hacks 101: 7 Summer Hacks That Actually Work in 40°C Heat -
 8 Workouts That Should Be a Part of Everyone’s Lifestyle for Longevity
8 Workouts That Should Be a Part of Everyone’s Lifestyle for Longevity
Cystitis: Causes and Treatments
Cystitis is somewhat a general lower urinary tract infection. It occurs mainly as an inflammation of the bladder wall. Though cystitis is not normally a disease leading to serious conditions in a patient, it can be rather uncomfortable and if left as such without any treatment may lead to complications.
Cystitis generally is seen in a patient when the urethra and bladder, which are normally unproductive, or free from microorganisms, are infected with bacteria. Bacteria attach to the layering of the bladder and the area becomes irritated and swollen.

Cystitis is more seen among females than males because women have shorter urethras. Around 80 percent of all urinary tract infections (UTIs) occur because of the result of bacteria from the bowel that reach the urinary tract.
Majority of these bacteria form part of the healthy intestinal flora, but once they enter the unproductive space in the urethra and bladder, they can cause a urinary tract infection. Cystitis in most cases is caused by a bacterial infection. Generally, mild cystitis will be cured within a few days. However, if it persists for more than 4 days, an opinion of a medical practitioner is necessitated.
Causes Of Cystitis
Several causes are responsible for the occurrence of cystitis. Let us discuss them:
1. Tampon and catheter usage: During tampon usage, when a tampon is inserted then there is a slight risk of bacteria entering through the pathway of the urethra. Inserting, changing, or prolonged use of a urinary catheter will lead to a possibility that the catheter will carry the bacteria along the urinary tract.
2. Diaphragm to control birth: There's a higher probability of cystitis to occur in women, who use the diaphragm with spermicides, in comparison to sexually active women who don't use that.
3. Full bladder: If the urinary bladder is not emptied completely and properly, it creates an environment for the multiplication of bacteria. This is usually very common among pregnant women or men whose prostates are enlarged.
4. Sexual activity: Sexually active women are generally at a higher risk of suffering from this condition because of bacteria entering through the pathway of the urethra.
5. Frequent or vigorous sex: This increases the chances of physical damage, which in turn increases the likelihood of occurence of cystitis. This is popularly called honeymoon cystitis.
6. Falling estrogen levels: During menopause, when the estrogen levels drop, the lining and layering of a woman's urethra becomes thinner. The thinner the lining becomes, the higher the chances are of infection and damage. Hence, after menopause the risk is definitely higher.
7. Gender: A woman's urethra opens near the anus, so there is a higher risk of bacteria from the intestines entering the urethra.
8. Mucus reduction: During menopause, women produce less mucus in the vaginal area. This mucus normally acts as a protective layer against bacteria.
9. Radiotherapy: Damage to the bladder because of radiotherapies can cause late radiation cystitis.
10. Blockage in the urinary system: Any blockage in the urinary system which prevents the urine's flow can cause this condition. Other bladder or kidney problems are also responsible for this condition.

Treatment Of Cystitis
Majority of cases of mild cystitis will get cured on its own within a few days. Cystitis that lasts for more than 4 days should require an opinion of the medical practitioner. The medical practitioners may prescribe a three or seven to ten-day course of antibiotics, depending on the patient. This should start to cure all the symptoms within a day.
If the symptoms do not improve after taking the antibiotics, the patient should return to his or her medical practitioner. In older people and those with weakened immune systems, there is a higher risk of the infection spreading to the kidney and thus leading to other complications.
Pregnant women should be properly taken care of and should be treated promptly if any symptoms of cystitis are found in those women. Generally used antibiotics for bacterial cystitis are trimethoprim-sulfamethoxazole, nitrofurantoin, ciprofloxacin, amoxicillin, levofloxacin, and cephalosporins.
Disclaimer: The information provided in this article is for general informational and educational purposes only and is not intended as a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or a qualified healthcare provider with any questions you may have regarding a medical condition.



 Click it and Unblock the Notifications
Click it and Unblock the Notifications
