Latest Updates
-
 Buttermilk Recipe: Your Cooling Summer Drink Essential
Buttermilk Recipe: Your Cooling Summer Drink Essential -
 Horoscope for Today May 14, 2026 - Small Choices, Big Impact
Horoscope for Today May 14, 2026 - Small Choices, Big Impact -
 Prateek Yadav Postmortem Reveals Six Injury Marks, Pulmonary Thromboembolism Reported As Cause Of Death
Prateek Yadav Postmortem Reveals Six Injury Marks, Pulmonary Thromboembolism Reported As Cause Of Death -
 Spicy Italian Classic Arrabiata Pasta Recipe: A Fiery Delight
Spicy Italian Classic Arrabiata Pasta Recipe: A Fiery Delight -
 Cannes 2026: Alia Bhatt’s Lace Umbrella Made Her Corset Saree Look Feel Straight Out Of Vintage Cinema
Cannes 2026: Alia Bhatt’s Lace Umbrella Made Her Corset Saree Look Feel Straight Out Of Vintage Cinema -
 Reels, Resentment And A Family That Broke Apart: What The Panipat Case Says About Modern India
Reels, Resentment And A Family That Broke Apart: What The Panipat Case Says About Modern India -
 Aloo Vada Recipe: Your Ultimate Crispy Street Snack
Aloo Vada Recipe: Your Ultimate Crispy Street Snack -
 Meet Sheema Kermani: Pakistani Classical Dancer and Activist Detained During Aurat March Protest
Meet Sheema Kermani: Pakistani Classical Dancer and Activist Detained During Aurat March Protest -
 CBSE 12th Result 2026 Declared Today: Pass Percentage, Toppers, and Full Guide
CBSE 12th Result 2026 Declared Today: Pass Percentage, Toppers, and Full Guide -
 Vat Savitri Vrat 2026: 16th or 17th May? Significance, Vrat Katha, Rituals And Why Married Women Observe It
Vat Savitri Vrat 2026: 16th or 17th May? Significance, Vrat Katha, Rituals And Why Married Women Observe It
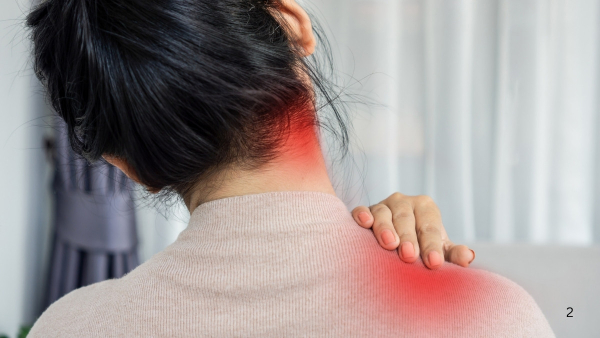
Knots, Aches, and Referred Pain: The Fascial Pain Syndrome Nobody Warned You About
She had been managing the ache in her shoulders for months, writing it off as desk tension. Then came the neck stiffness, the throbbing at the base of her skull, and a nagging discomfort that shifted - inexplicably - from her back to her jaw. No injury. No obvious cause.
For many women, this kind of chronic, shape-shifting pain is disturbingly familiar - and far too often dismissed as "just stress." But behind these symptoms may lie a culprit most people have never heard of: the fascia. A thin, tough sheet of connective tissue that envelops muscles, organs, nerves, and bones throughout the body, fascia plays a far larger role in chronic pain than medicine has traditionally acknowledged.
Dr Sandhya Manorenj, Senior Consultant, Department of Neurology, KIMSHEALTH, Thiruvananthapuram, explains why women bear a disproportionate burden of fascial pain, and what can actually be done about it.
Impact Of Fascial Pain
"Fascial pain can contribute to chronic pain, fatigue, and reduced quality of life, especially among women. Among them, the fascia around the muscle is most affected, leading to Myofascial Pain Syndrome. It involves some muscles and the thin cover of tissue that holds muscles in place, called fascia," explained Dr Manorenj. Pressure on these areas, called trigger points, causes pain. Sometimes, the pain is felt in other parts of the body. This is called referred pain. The pain is often felt as shoulder pain, back pain, tension headaches and face pain.
Types of Myofascial Pain
Myofascial pain can be divided into two categories: acute and chronic. Acute myofascial pain syndrome may settle on its own or through simple treatments, while chronic myofascial pain syndrome can last for six months or even longer. "Myofascial pain is widespread, with estimates suggesting that up to 85% of people experience it at some point in their lives. While it affects both men and women, research shows that around 65% of middle-aged women are affected by myofascial pain syndrome," added Dr Manorenj.
Common Symptoms of Fascial Pain
- Deep, aching muscular pain
- Pain that migrates from one area to another or that doesn't go away or gets worse.
- Tender knots in the muscles
- Trouble sleeping due to pain
- Headaches or jaw discomfort
- Pain exacerbated by stress or prolonged positions
- Reduced flexibility and movement
- A general feeling of not being well
Why Women Are at Greater Risk
While myofascial pain syndrome affects both men and women, research tells a telling story: around 65% of middle-aged women are affected. That disproportionate burden is not coincidental.
Dr Manorenj outlines several interconnected factors that make women more vulnerable.
- Hormonal Fluctuations: Changes in oestrogen - across the menstrual cycle, during pregnancy, and through menopause - can significantly heighten pain sensitivity, making fascia and muscle tissue more reactive to stress and inflammation.
- Differences in Pain Perception: Research indicates that women may process pain differently at a neurological level, increasing their susceptibility to chronic pain conditions.
- Joint Hypermobility: Women tend to have more flexible joints. While this can be an advantage in certain contexts, it also places additional stress on fascia and surrounding muscle tissue.
- Work and Lifestyle Demands: Women who manage both professional and domestic responsibilities, often simultaneously, face prolonged periods of standing, poor posture, inadequate rest, and insufficient recovery time. The body, eventually, registers the cost.
- Autoimmune Conditions: Many autoimmune diseases, including rheumatoid arthritis and lupus, are significantly more common in women. These conditions can overlap with and amplify fascial pain.
Effective Ways to Manage Fascial Pain
The good news is that fascial pain can often be managed successfully through a combination of movement, therapy, and lifestyle adjustments.
Physical Movement and Therapy
Activities that improve flexibility and circulation can help reduce stiffness and pain, including:
- Stretching
- Yoga
- Pilates
- Walking
- Physiotherapy
Manual and Targeted Therapies
Specific therapies may help release tension within fascia and muscles, such as:
- Myofascial release therapy
- Massage therapy
- Foam rolling
- Dry needling
- Trigger point therapy
Stress Management and Rest
Mental stress can worsen muscular tension and pain. Practices like meditation, breathing exercises, and proper sleep are equally important in recovery.
Nutrition and Hydration
Staying hydrated and following a balanced diet can support tissue health and reduce inflammation. Foods rich in:
- Fruits and vegetables
- Protein
- Omega-3 fatty acids
may help support overall recovery and pain management.
Disclaimer: The information provided in this article is for general informational and educational purposes only and is not intended as a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or a qualified healthcare provider with any questions you may have regarding a medical condition.



 Click it and Unblock the Notifications
Click it and Unblock the Notifications