Latest Updates
-
 Authentic Indian Style Arrabiata Pasta Recipe
Authentic Indian Style Arrabiata Pasta Recipe -
 Saree, But Make It Denim: Madhuri Dixit’s Denim Saree Look Breaks The Internet
Saree, But Make It Denim: Madhuri Dixit’s Denim Saree Look Breaks The Internet -
 Think Twice Before Eating Street Food Wrapped In Newspaper, FSSAI Issues Warning
Think Twice Before Eating Street Food Wrapped In Newspaper, FSSAI Issues Warning -
 Pride Month 2026: Inspiring LGBTQIA+ Firsts In India That Built Visibility, Representation And Change
Pride Month 2026: Inspiring LGBTQIA+ Firsts In India That Built Visibility, Representation And Change -
 World Food Safety Day 2026: Can Carrot Extract Help Fake Ghee Evade Detection? An IIT-BHU Study Reveals How
World Food Safety Day 2026: Can Carrot Extract Help Fake Ghee Evade Detection? An IIT-BHU Study Reveals How -
 Easy Aloo Posto Recipe: A Bengali Lunch Delight
Easy Aloo Posto Recipe: A Bengali Lunch Delight -
 Who Was Salim Kumar? The National Award Winner Behind Countless Laughs Passes Away At 56
Who Was Salim Kumar? The National Award Winner Behind Countless Laughs Passes Away At 56 -
 Adhik Bhanu Saptami 2026: Significance, Puja Vidhi, Surya Mantras And The Role Of Ravi Yoga And Adhik Maas
Adhik Bhanu Saptami 2026: Significance, Puja Vidhi, Surya Mantras And The Role Of Ravi Yoga And Adhik Maas -
 Gujarati Style Aamras Recipe: A Taste of Summer Breakfast
Gujarati Style Aamras Recipe: A Taste of Summer Breakfast -
 World Food Safety Day 2026: Date, Theme, History, Significance, and Everything You Need to Know
World Food Safety Day 2026: Date, Theme, History, Significance, and Everything You Need to Know
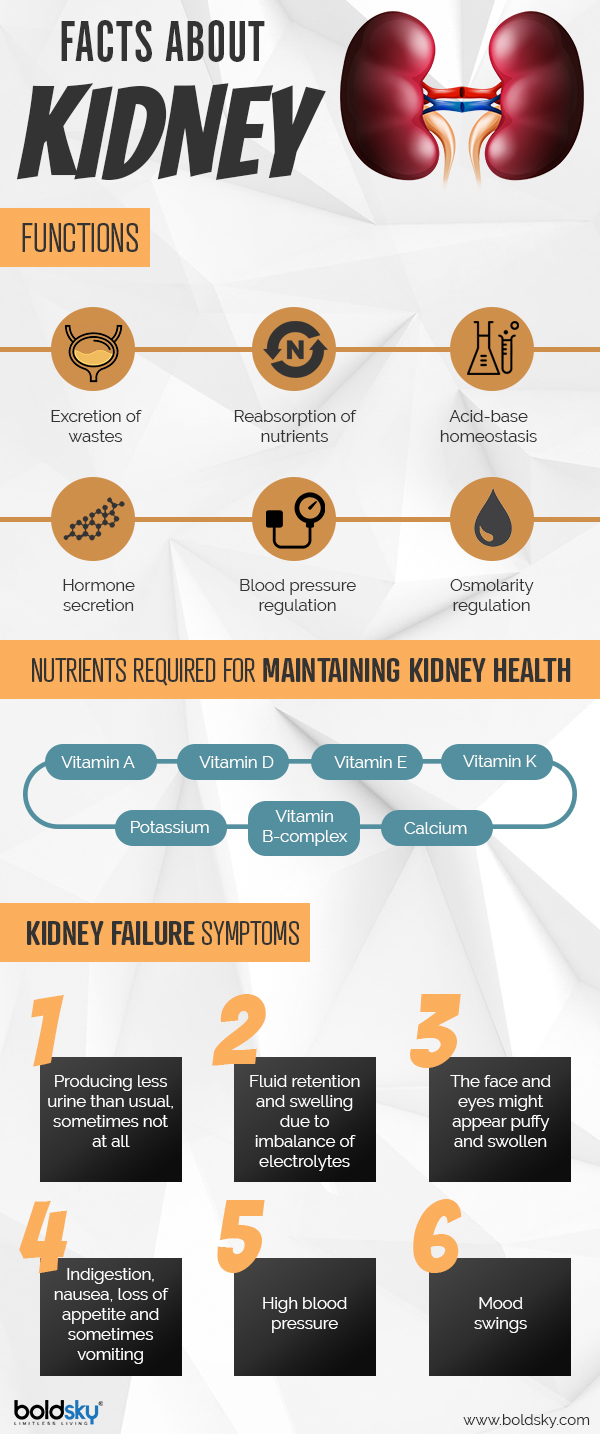
World Kidney Day: Everything You Need To Know About Renal Replacement Therapy
In cases of acute kidney insufficiency (AKI) [1] , a treatment method needs to be deployed that can treat the progressive deterioration in the regulation of the body's acid-base balance along with the electrolyte and fluid balance [2] . Renal replacement therapy (RRT) can successfully replace the waste filtering functions of a normal kidney. For people suffering from conditions such as AKI, RRT is extremely necessary to assist the body such that it can deal with the ensuing metabolic activities [3] .
Researchers are of the opinion that RRT should be called 'renal support therapy' instead, as dialysis (most common RRT) is not the ultimate treatment option, as it cannot compensate for some of the tasks performed by the kidney [4] .

On this World Kidney Day (14 March), read on to know more about RRT. The criteria behind initiating it and the associated complications that can arise.
What Is Renal Replacement Therapy (RRT)?
RRT is a therapy that is used as a substitute for the normal blood-filtering functionality of the kidneys [5] . This therapy is used when the kidneys do not work well (especially in cases of renal failure, for instance in the case of acute kidney injury or chronic kidney disease).
Usually, RRT is facilitated through methods that include dialysis [6] , haemofiltration [7] and haemodiafiltration [8] . These methods aim at filtering blood with or without machines. In certain cases, RRT also involves kidney transplantation [9] (although this serves to be the ultimate form of replacement of the old kidney with that of a donor's kidney).
Use of RRT cannot be referred to as a cure for kidney disease. They are basically life-extending treatments. Early dialysis in cases of acute renal failure has shown favourable outcomes in most cases.
Indications For Renal Replacement Therapy (RRT)
Situations which result in the kidney functionality failing to achieve homeostasis (stable equilibrium between interdependent elements) would require the use of RRT [10] . Such situations are as follows:
- Septic shock (organ injury or damage due to an infection that leads to low blood pressure and abnormalities in cellular metabolism) [11]
- Acute kidney insufficiency [12]
- Chronic renal failure [13]
- Myasthenia gravis (chronic autoimmune neuromuscular disease) [14]
- Acute hepatic failure superimposed or chronic failure [15]
Modes Of Renal Replacement Therapy (RRT)
The following are the different techniques used for performing RRT:
- Intermittent Haemodialysis (IHD) [16] : This is associated with hypotension and allows only intermittent removal of wastes.
- Continuous RRT (CRRT) [17] : This is a costly and complex procedure. This helps in avoiding hypotensive episodes and requires continuous anticoagulation therapy (a therapy that uses anticoagulants to reduce the body's ability to form blood clots).
- Peritoneal dialysis [18]
- Plasmapheresis or plasma exchange [19]
Some units use hybrid therapies - a combination of IHD and CRRT. This is commonly known as 'slow low-efficiency daily dialysis' [20] .
Criteria For Renal Replacement Therapy (RRT)
Initiating RRT is based on the below criteria [21] :
- Insufficient urine output (oliguria)
- Absence of urine production (anuria)
- Metabolic acidosis without compensation
- High serum creatinine and urea levels above fixed criteria
- Temperature above 40 degree Celsius
- Cardiac failure
- Lithium overdose
- Hypothermia (abnormally low body temperature)
- Dangerous fluctuations in serum sodium and potassium
- Pulmonary oedema (fluid buildup in the lungs) that has turned non-responsive to diuretic therapy (reducing the amount of salt and water in the body)
- High levels of blood urea
- Patients who possess the risk of pulmonary oedema and cannot tolerate volume infusions even when there is a need for the infusion of large amounts of fluid or blood
The above-mentioned criteria are based on opinions from experts rather than on evidence from randomized controlled trials.
The Principle Of Renal Replacement Therapy (RRT)
RRT aims at doing the following [22] :
- Solute and water removal
- Correction of electrolyte abnormalities
- Normalization of acid-base disturbances
In RRT, a semi-permeable membrane is used to filter out the wastes by diffusion (haemodialysis) [23] or convection (haemofiltration) [24] along with excessive water. The filtered wastes are in the form of solutes. This procedure is referred to as ultrafiltration. The rate at which ultrafiltration is done is dependent on the transmembrane pressure and the permeability of the membrane [25] .
The diffusion of the solute is dependent on the following factors [26] :
- Temperature
- Diffusion coefficient
- Surface area of the membrane
- The inter-compartment concentration gradient that is separated by the membrane
- Characteristics of the solute: protein-binding, molecular weight, flow rate of the blood and dialysate flow
Process of haemodialysis [27] : Diffusion across the membrane allows for solute clearance. Within the filter, the space outside the blood-containing fibres is filled with dialysate. This is pumped in a counter-current fashion to the flow of blood. Dialysate is reconstituted to contain a buffer and electrolytes that are dissolved in water (devoid of impurities and toxins). The counter-current flow system helps in maintaining a waste-solute concentration gradient.
Process of haemofiltration [28] : This is a convective process. A hydrostatic pressure gradient is used to filter water, solute and plasma across a membrane. The mechanism is called 'solute drag' wherein molecules of appropriate sizes are pulled along with the mass movement of the solvent [29] (otherwise called ultrafiltration). The direction and magnitude of the transmembrane pressure determine the convective transport. When the flow rate is high, ultrafiltration production is increased, which in turn increases the solute clearance. On the other hand, measures that increase the negative pressure also show a marked effect. The discarded fluid is called effluent. When such high volumes are produced, the volume circulating in the patient is replaced with a crystalloid, balanced buffer solution.
Mechanism Of Different Modes Of Renal Replacement Therapy (RRT)
Haemofiltration involves removal of water by a transmembrane pressure that is above the oncotic pressure of the plasma [30] .
In the case of peritoneal dialysis, the osmolarity of the dialysate is increased for water removal [31] .
Intermittent haemodialysis [32] follows the mechanism quite similar to haemofiltration and is made up of three parts [33] :
- The dialysate
- The dialyzer
- The blood delivery system
Complications Of Renal Replacement Therapy (RRT)
The problems that can arise during RRT are [34]
- mechanical complication of the extracorporeal circuit (apparatus carrying the blood outside the patient's body),
- catheter-related complications (such as infection, failure of access, blood loss and disconnection),
- activation of the coagulation cascade (events that lead to haemostasis) and
- fluctuations in the salt-water balance.
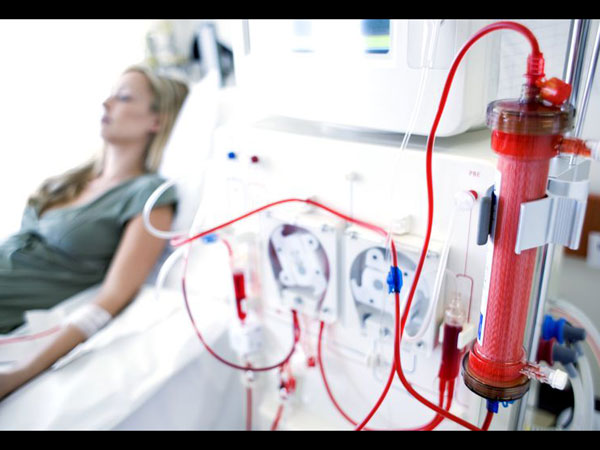
The following are the complications specific to haemodialysis [35] :
- Muscle cramps
- Hypotension (low blood pressure)
- Complications during transport
- Cardiac arrest
- Air embolism (a blood vessel blockage caused by one or more bubbles of air or other gas in the circulatory system)
- Venous thrombosis (blood clot within a vein)
- Accidental removal of tubes (connections to a ventilator, dialysis catheters/airway tubes)
- Infections
- Coagulopathy (the blood's ability to coagulate is impaired)
- Anaphylactoid reactions to the dialyzer
- Deterioration of haemodynamic status (due to the removal of drugs used for treating underlying conditions, cardiac arrhythmias)
- Obstruction of dialysis catheters/blood vessels
The following are the complications specific to peritoneal dialysis [36] :
- Protein loss
- Peritonitis (inflammation of the peritoneum)
- Hyperglycemia (high blood sugar)
- Catheter-associated infections
On A Final Note...
The downsides of RRT must be balanced against its benefits. It is also important that experts treating the patient give consideration to the fact that spontaneous recovery of the kidneys may occur. Experts should base the decision to institute RRT after considering the severity of other organ failure and the trajectory of the person's illness [37] .
RRT is ideally continued until the patient begins to show evidence of native renal functionality. The first recovery sign is usually an increase in the urine output. A progressive decline in serum creatinine during steady-state is also an indication of recovery [38] .
Disclaimer: The information provided in this article is for general informational and educational purposes only and is not intended as a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or a qualified healthcare provider with any questions you may have regarding a medical condition.
Observational studies have reported that initiating RRT in the early stages correlates with improved survival [39] .
- [1] Makris, K., & Spanou, L. (2016). Acute Kidney Injury: Definition, Pathophysiology and Clinical Phenotypes.The Clinical biochemist. Reviews,37(2), 85-98.
- [2] Goyal A, Bashir K. Acute Renal Failure. [Updated 2019 Jan 21]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2018 Jan.
- [3] Palevsky P. M. (2013). Renal replacement therapy in acute kidney injury.Advances in chronic kidney disease,20(1), 76-84.
- [4] Vadakedath, S., & Kandi, V. (2017). Dialysis: A Review of the Mechanisms Underlying Complications in the Management of Chronic Renal Failure.Cureus,9(8), e1603.
- [5] Liu, K. D., & Palevsky, P. M. (2016). RRT in AKI: Start Early or Wait?.Clinical journal of the American Society of Nephrology : CJASN,11(10), 1867-1871.
- [6] Lin, Z. H., & Zuo, L. (2015). When to initiate renal replacement therapy: The trend of dialysis initiation.World journal of nephrology,4(5), 521-527.
- [7] Mirrakhimov, A. E., Barbaryan, A., Gray, A., & Ayach, T. (2016). The Role of Renal Replacement Therapy in the Management of Pharmacologic Poisonings.International journal of nephrology,2016, 3047329.
- [8] Qureshi, A. R., Evans, M., Stendahl, M., Prütz, K. G., & Elinder, C. G. (2013). The increase in renal replacement therapy (RRT) incidence has come to an end in Sweden-analysis of variations by region over the period 1991-2010.Clinical kidney journal,6(3), 352-357.
- [9] Abecassis, M., Bartlett, S. T., Collins, A. J., Davis, C. L., Delmonico, F. L., Friedewald, J. J., Hays, R., Howard, A., Jones, E., Leichtman, A. B., Merion, R. M., Metzger, R. A., Pradel, F., Schweitzer, E. J., Velez, R. L., … Gaston, R. S. (2008). Kidney transplantation as primary therapy for end-stage renal disease: a National Kidney Foundation/Kidney Disease Outcomes Quality Initiative (NKF/KDOQITM) conference.Clinical journal of the American Society of Nephrology : CJASN,3(2), 471-480.
- [10] Deepa, C., & Muralidhar, K. (2012). Renal replacement therapy in ICU.Journal of anaesthesiology, clinical pharmacology,28(3), 386-396.
- [11] Chen, Y. Y., Wu, V. C., Huang, W. C., Yeh, Y. C., Wu, M. S., Huang, C. C., Wu, K. D., Fang, J. T., Wu, C. J., NSARF, CAKS Group (2018). Norepinephrine Administration Is Associated with Higher Mortality in Dialysis Requiring Acute Kidney Injury Patients with Septic Shock.Journal of clinical medicine,7(9), 274.
- [12] Romagnoli, S., & Ricci, Z. (2016). When to start a renal replacement therapy in acute kidney injury (AKI) patients: many irons in the fire.Annals of translational medicine,4(18), 355.
- [13] De Corte, W., Dhondt, A., Vanholder, R., De Waele, J., Decruyenaere, J., Sergoyne, V., Vanhalst, J., Claus, S., … Hoste, E. A. (2016). Long-term outcome in ICU patients with acute kidney injury treated with renal replacement therapy: a prospective cohort study.Critical care (London, England),20(1), 256.
- [14] Jordan, A., & Freimer, M. (2018). Recent advances in understanding and managing myasthenia gravis.F1000Research,7, F1000 Faculty Rev-1727.
- [15] Anand, A. C., & Dhiman, R. K. (2016). Acute on Chronic Liver Failure-What is in a 'Definition'?.Journal of clinical and experimental hepatology,6(3), 233-240.
- [16] Intermittent haemodialysis. (1966).British medical journal,1(5501), 1433-1434.
- [17] Jaryal, A., & Vikrant, S. (2017). A Study of Continuous Renal Replacement Therapy and Acute Peritoneal Dialysis in Hemodynamic Unstable Patients.Indian journal of critical care medicine : peer-reviewed, official publication of Indian Society of Critical Care Medicine,21(6), 346-349.
- [18] Centre for Clinical Practice at NICE (UK). Peritoneal Dialysis: Peritoneal Dialysis in the Treatment of Stage 5 Chronic Kidney Disease. London: National Institute for Health and Clinical Excellence (UK); 2011 Jul. (NICE Clinical Guidelines, No. 125.)
- [19] Linker C. (1983). Plasmapheresis in clinical medicine.The Western journal of medicine,138(1), 60-69.
- [20] Fieghen, H. E., Friedrich, J. O., Burns, K. E., Nisenbaum, R., Adhikari, N. K., Hladunewich, M. A., Lapinsky, S. E., Richardson, R. M., Wald, R., University of Toronto Acute Kidney Injury Research Group (2010). The hemodynamic tolerability and feasibility of sustained low efficiency dialysis in the management of critically ill patients with acute kidney injury.BMC nephrology,11, 32.
- [21] Kipnis, E., Garzotto, F., & Ronco, C. (2016). Timing of RRT initiation in critically-ill patients: time for precision medicine.Journal of thoracic disease,8(10), E1242-E1243.
- [22] Naka, T., & Bellomo, R. (2004). Bench-to-bedside review: treating acid-base abnormalities in the intensive care unit--the role of renal replacement therapy.Critical care (London, England),8(2), 108-114.
- [23] Deepa, C., & Muralidhar, K. (2012). Renal replacement therapy in ICU.Journal of anaesthesiology, clinical pharmacology,28(3), 386-396.
- [24] Palevsky P. M. (2013). Renal replacement therapy in acute kidney injury.Advances in chronic kidney disease,20(1), 76-84.
- [25] Ricci, Z., Romagnoli, S., & Ronco, C. (2016). Renal Replacement Therapy.F1000Research,5, F1000 Faculty Rev-103.
- [26] Mehta R. L. (2015). Challenges and pitfalls when implementing renal replacement therapy in the ICU.Critical care (London, England),19 Suppl 3(Suppl 3), S9.
- [27] Vadakedath, S., & Kandi, V. (2017). Dialysis: A Review of the Mechanisms Underlying Complications in the Management of Chronic Renal Failure.Cureus,9(8), e1603.
- [28] Davenport A. (2010). Adequacy of haemodialysis and or haemofiltration treatments for patients with acute kidney injury.F1000 medicine reports,2, 33.
- [29] Pannu, N., & Gibney, R. N. (2005). Renal replacement therapy in the intensive care unit.Therapeutics and clinical risk management,1(2), 141-150.
- [30] Bellomo, R., & Ronco, C. (2000). Continuous haemofiltration in the intensive care unit.Critical care (London, England),4(6), 339-345.
- [31] Ansari N. (2011). Peritoneal dialysis in renal replacement therapy for patients with acute kidney injury.International journal of nephrology,2011, 739794.
- [32] Gibney R. T. (2016). Continous renal replacement therapy and intermittent hemodialysis in acute kidney injury: equivalent or complementary?.Journal of thoracic disease,8(9), 2397-2399.
- [33] Sankarasubbaiyan, S., Janardan, J. D., & Kaur, P. (2013). Outcomes and characteristics of intermittent hemodialysis for acute kidney injury in an intensive care unit.Indian journal of nephrology,23(1), 30-33.
- [34] Jaryal, A., & Vikrant, S. (2017). A Study of Continuous Renal Replacement Therapy and Acute Peritoneal Dialysis in Hemodynamic Unstable Patients.Indian journal of critical care medicine : peer-reviewed, official publication of Indian Society of Critical Care Medicine,21(6), 346-349.
- [35] Kayalar, A. O., Basturk, T., Koc, Y., Yilmaz, F., Caglayan, F. B., Sakaci, T., Ahbap, E., … Ünsal, A. (2016). Comparison of Long-term Complications in Patients on Haemodialysis and Peritoneal Dialysis Longer than 10 Years.Journal of clinical and diagnostic research : JCDR,10(2), OC05-8.
- [36] Kim, J. E., Park, S. J., Oh, J. Y., Kim, J. H., Lee, J. S., Kim, P. K., & Shin, J. I. (2015). Noninfectious Complications of Peritoneal Dialysis in Korean Children: A 26-Year Single-Center Study.Yonsei medical journal,56(5), 1359-1364.
- [37] Legrand M. (2016). Should we apply "early" initiation of renal replacement therapy to critically ill patients with acute kidney injury?.Journal of thoracic disease,8(10), E1271-E1273.
- [38] Joannidis, M., & Forni, L. G. (2011). Clinical review: timing of renal replacement therapy.Critical care (London, England),15(3), 223.
- [39] Bhatt, G. C., & Das, R. R. (2017). Early versus late initiation of renal replacement therapy in patients with acute kidney injury-a systematic review & meta-analysis of randomized controlled trials.BMC nephrology,18(1), 78.



 Click it and Unblock the Notifications
Click it and Unblock the Notifications
