Latest Updates
-
 Horoscope for Today April 25, 2026 - Steady Steps, Clear Focus, Practical Gains
Horoscope for Today April 25, 2026 - Steady Steps, Clear Focus, Practical Gains -
 Rich Mughlai Special Chicken Korma Recipe
Rich Mughlai Special Chicken Korma Recipe -
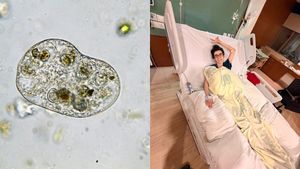 A Hidden Foodborne Infection: What You Should Know About Cyclospora
A Hidden Foodborne Infection: What You Should Know About Cyclospora -
 Melt-in-Mouth Sweet Mysore Pak Recipe: A Classic Indian Delight
Melt-in-Mouth Sweet Mysore Pak Recipe: A Classic Indian Delight -
 Between Meetings and Meals: Why American Pecans Are the Ideal Midday Snack
Between Meetings and Meals: Why American Pecans Are the Ideal Midday Snack -
 Skincare Hacks 101: 7 Summer Hacks That Actually Work in 40°C Heat
Skincare Hacks 101: 7 Summer Hacks That Actually Work in 40°C Heat -
 8 Workouts That Should Be a Part of Everyone’s Lifestyle for Longevity
8 Workouts That Should Be a Part of Everyone’s Lifestyle for Longevity -
 Simple Everyday Dal Recipe: Your Go-To Chana Dal
Simple Everyday Dal Recipe: Your Go-To Chana Dal -
 Italian PM Giorgia Meloni’s ‘Desi’ Look Wins Internet with Jhumkas
Italian PM Giorgia Meloni’s ‘Desi’ Look Wins Internet with Jhumkas -
 May 2026 Bank Holidays in India: Check Complete State-Wise List
May 2026 Bank Holidays in India: Check Complete State-Wise List
Mydriasis (Dilated Pupils): Causes, Symptoms, Diagnosis And Treatment
Your pupils help you perceive light and darkness. The pupils dilate when the surroundings are dim so that more light can enter your eyes. And mydriasis is the condition that causes the pupils to dilate without any change in the levels of light.

So, mydriasis is the medical term for defining the unusual dilation or widening of the pupils. Normally, the pupils dilate or widen as a response to low light so they can collect more light and in some people, the pupils can dilate without any relation to the levels of light [1] [2] .
Causes Of Mydriasis
Various factors can develop the condition in an individual and they are mentioned below[3] [4] .
- Medications: Use of certain medications such as antihistamines, botox, muscle relaxants, and drugs used to treat Parkinson's disease may cause the pupils to dilate.
- Plants: Some plants like Jimson weed or angel's trumpet can cause the pupils to dilate.
- Injury to the eye: Injuries such as a blunt force trauma can damage the nerves that control the pupils, which can disrupt the normal pupil response to levels of light.
- Increased oxytocin: High levels of oxytocin can cause temporary dilation of the pupils. The hormone is released when there are social or physical interactions with other people.
- Drug use: Using drugs such as ecstasy, cocaine, hallucinogenics, and crystal methamphetamine can lead to mydriasis. Drugs like LSD affect the serotonin receptors in the brain, thereby causing your pupils to dilate.
- Benign episodic unilateral mydriasis (BEUM): It is a temporary condition that causes only one of your pupils to dilate. This condition can also cause mild headache, eye pain, light sensitivity, and blurred vision [5] .
- Cranial nerve neuropathy: It is the gradual damage of the nerves that connect the eye. The oculomotor nerve is responsible for the constriction and dilation of the pupils and damage to this can result in mydriasis [6] .
- Traumatic brain injury: Injuries to your brain can cause increased intracranial pressure, which can have a direct impact on the pupils.

Symptoms Of Mydriasis
The characteristic symptom of the condition is dilated pupils that do not get bigger or smaller. And when your pupils are dilated, it can become difficult to see properly - thereby resulting in blurry vision [7] .
One may also experience headaches, dizziness, eye irritation and trouble sleeping.
Diagnosis Of Mydriasis
The symptoms and the medical history of the patient will be reviewed. The doctor will ask about the use of medications or drugs, and whether you have had any eye injuries.
The diagnosis may be comprised of a visual acuity test and an ocular motility test, to examine the muscles of your eye [8] [9] .
For some individuals, a blood test may be advised.
Treatment For Mydriasis
The method of treatment adopted for the condition will be dependent on the cause. Mostly, opaque contact lenses or light-sensitive sunglasses will be prescribed by the doctor [10] .
If pupil dilation is caused by a reaction to the medication, then doctors would recommend you to wait it out; even though several drugs could quickly get the pupils back to normal size.
In rare cases, surgery may be required (for mydriasis caused by injuries to the brain and eyes).
Managing Mydriasis
Apart from the treatment measures, there are some ways through which you can control the symptoms of the dilated pupils [11] [12] .
- Avoid reading the text too close to your eyes
- Avoid direct sunlight
- Use sunglasses prescribed by an optometrist in bright environments
- Avoid driving, especially during the day
Disclaimer: The information provided in this article is for general informational and educational purposes only and is not intended as a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or a qualified healthcare provider with any questions you may have regarding a medical condition.
- [1] Al-Zubidi, N., & Lee, A. G. (2016). Benign Episodic Pupillary Mydriasis. Encyclopedia of Ophthalmology, 1-2.
- [2] Sánchez-de la Torre, J. R., Drake-Pérez, M., Casado, A., Palacio-Portilla, E. J., Revilla, M., Vázquez-Higuera, J. L., & Infante, J. (2019). Persistent isolated mydriasis as an early sign of internal carotid artery dissection: Pourfour du petit syndrome. Clinical neurology and neurosurgery, 182, 70-72.
- [3] Woreta, F. A., Mir, T. A., & Jampel, H. (2017). Pharmacologic interventions for mydriasis in cataract surgery. Cochrane Database of Systematic Reviews, (10).
- [4] Riehani, A., & Pahwa, R. (2016). 1850: UNILATERAL PUPILLARY MYDRIASIS FROM IPRATROPIUM BROMIDE: A FALSE SIGN OF STROKE. Critical Care Medicine, 44(12), 538.
- [5] Fukuo, M., Kondo, M., Hirose, A., Fukushima, H., Ikesugi, K., Sugimoto, M., ... & Kitano, S. (2016). Screening for diabetic retinopathy using new mydriasis-free, full-field flicker ERG recording device. Scientific reports, 6, 36591.
- [6] Chamberlain, P. D., Sadaka, A., Berry, S., & Lee, A. G. (2018). Intermittent mydriasis associated with carotid vascular occlusion. Eye, 32(2), 457.
- [7] Lam, S., Guimaraes, C., & Jones, J. Y. (2017). Congenital Mydriasis With Aortic and Cerebrovascular Disease. Pediatric neurology, 74, 100-101.
- [8] Ma, M., & Liao, J. (2017). Unilateral Mydriasis: Emergent or Benign. Proceedings of UCLA Healthcare, 21.
- [9] Stevenson, A., Yoganathan, K., Fox, J., & Shackleton, D. (2019). Challenging case of unilateral mydriasis. Emerg Med J, 36(4), 201-218.
- [10] Liu, H., Ji, X., Dhaliwal, S., Rahman, S. N., McFarlane, M., Tumber, A., ... & Westall, C. (2018). Evaluation of light-and dark-adapted ERGs using a mydriasis-free, portable system: clinical classifications and normative data. Documenta Ophthalmologica, 137(3), 169-181.
- [11] Pennington, K. M., & Louis, E. K. S. (2016). “Don't Believe Your Eyes” Ipratropium Induced Mydriasis: A Case Report and Review of the Literature. General medicine (Los Angeles, Calif.), 4(3).
- [12] Korf, E. M., Tronnier, V. M., Gliemroth, J., & Küchler, J. N. (2017). Isoflurane-Associated Mydriasis Mimicking Blown Pupils in a Patient Treated in a Neurointensive Care Unit. Journal of Neurological Surgery Part A: Central European Neurosurgery, 78(04), 403-406.



 Click it and Unblock the Notifications
Click it and Unblock the Notifications
