Latest Updates
-
 Paneer Lababdar Recipe: Your Restaurant-Style Finish
Paneer Lababdar Recipe: Your Restaurant-Style Finish -
 Mouni Roy’s Cannes 2026 Patola Gown Took 300 Hours To Craft — The Story Of Gujarat’s GI-Tagged Weave
Mouni Roy’s Cannes 2026 Patola Gown Took 300 Hours To Craft — The Story Of Gujarat’s GI-Tagged Weave -
 Bread Pizza Recipe: Your Instant Snack Hack
Bread Pizza Recipe: Your Instant Snack Hack -
 India's Hottest City Hit 47.6°C Today — This Is What Heatstroke Looks Like
India's Hottest City Hit 47.6°C Today — This Is What Heatstroke Looks Like -
 Exclusive: Rubina Dilaik Said Yes To The Ward In Seconds: Here's The Raw Truth Behind Why
Exclusive: Rubina Dilaik Said Yes To The Ward In Seconds: Here's The Raw Truth Behind Why -
 PM Modi Turns Viral ‘Melodi’ Nickname Real With Melody Gift To Meloni, Inside India’s Iconic Toffee Origin
PM Modi Turns Viral ‘Melodi’ Nickname Real With Melody Gift To Meloni, Inside India’s Iconic Toffee Origin -
 Superglue, A Potato, A Plastic Bag: The Dangerous DIY Contraception Cases That Shocked Doctors
Superglue, A Potato, A Plastic Bag: The Dangerous DIY Contraception Cases That Shocked Doctors -
 One Pot Easy Meal: Delicious Veg Pulav Recipe
One Pot Easy Meal: Delicious Veg Pulav Recipe -
 'Melodi' Moment Breaks The Internet: PM Modi Meets Giorgia Meloni In Rome, Colosseum Diplomacy Explained
'Melodi' Moment Breaks The Internet: PM Modi Meets Giorgia Meloni In Rome, Colosseum Diplomacy Explained -
 Remembering Bipin Chandra Pal On His 94th Death Anniversary With 10 Bold Quotes On Swaraj And Identity
Remembering Bipin Chandra Pal On His 94th Death Anniversary With 10 Bold Quotes On Swaraj And Identity
Uterine Polyps (Endometrial Polyps): Symptoms, Causes & Treatment
Also termed as endometrial polyps, these are specific growths attached to the inner walls of the uterus. It develops in the form of a mass and extends into the uterine cavity. The uterine polyps are the result of the overgrowth of cells in the [1] endometrium. The polyps are attached to the uterus by an elongated pedicle, a small stalk-like structure.
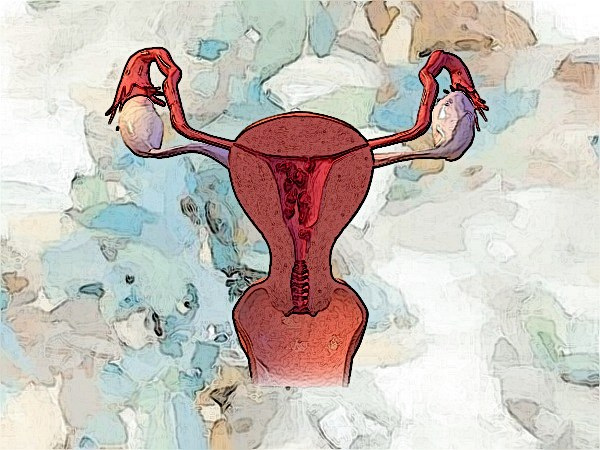
The small growths develop in the womb or uterus. The size of polyps can vary, and a single person can develop more than one polyp. The polyps are usually [2] non-cancerous and benign, but in some cases, it can develop into cancer, termed as precancerous polyps. Generally, polyps are contained within the uterus but it can also slip down through the cervix and into the vagina.
Uterine polyps are commonly found in [3] women going through or have finished menopause. But in rare cases, it is found in younger women. Obesity and anti oestrogen drugs can also cause uterine polyps.
Symptoms Of Uterine Polyps
The small growth that develops inside your uterus has the following [4] signs.
- Irregular menstrual bleeding (having frequent and unpredictable periods)
- Bleeding or spotting between [5] menstrual periods
- Unusual excessive flow during menstrual periods
- Vaginal bleeding or spotting after menopause
- Infertility.
Causes Of Uterine Polyps
There is an uncertainty pertaining to the factor that develops the small [6] growths in the uterus.
Some of the studies suggested changes in the hormone levels to be the cause of uterine polyps. Each month, the oestrogen levels in your body rise and falls. This causes the lining of your uterus to thicken and shed during your menstrual period. The constant changes in the hormone levels each month could act as a reason causing the growth of uterine polyps.
Age is regarded as another factor that can [7] act as a factor causing the growth of polyps. Between the age of 40 to 50, women have a high chance of developing uterine polyps. This can be attributed to the changes affecting the oestrogen levels before and after one goes through menopause.
Some of the other causes of uterine polyps are as follows.[8]
- Clogged blood vessels.
- Obesity.
- High blood pressure.
- Chronic inflammation of the vagina, cervix or uterus.
- Certain medications such as the breast cancer drug tamoxifen.
- An increase in the levels of oestrogen.
Diagnosis Of Uterine Polyps
In order to examine and analyse the [9] condition, your doctor will ask you about your menstrual history. This will include questions involving how often you get your periods and how long it lasts. The doctor may perform the following tests to further examine the condition.
1. Hysteroscopy
The doctor will insert a flexible, thin telescope known as hysteroscope into your uterus, through your vagina and cervix. The procedure [10] will help the doctor examine the insides of your uterus.
2. Transvaginal ultrasound
Under this procedure, a slender device shaped like a wand will be placed in your vagina. It will emit sound waves, which will help in creating an image of the interior of the uterus. The ultrasound will detect if there are any polyp-like growth in the endometrial [11] tissue.
3. Sonohysterography
This will be conducted after the transvaginal ultrasound. Using a catheter (a thin tube), a sterile fluid will be introduced into your uterus. The fluid is used because it causes the uterus to expand, thus providing a clearer image of the insides [12] of the uterus. This will help in analysing and examining any growths present in the uterine cavity during the ultrasound procedure.
4. Endometrial biopsy
In this procedure, the doctor will use a suction catheter to collect a specimen from your uterus for further testing in the lab. The collected tissue [13] will be collected from the inner walls of the uterus. The sample will be sent to a lab to determine any possible abnormalities or growths.
5. Curettage
This procedure is carried out in an operating room. Currettage helps in diagnosing as well as treating polyps. A long instrument called [14] as the curette will be used by the doctor for the purpose of collecting tissue from the inner walls of your uterus. A small loop at the end of the curette helps the doctor in collecting the tissue or the polyps. The scrapped off tissue will be then sent to a laboratory, like endometrial biopsy, to determine the possible presence of cancer cells.
Treatment For Uterine Polyps
There are certain methods and steps used in treating the abnormal growth in the inner walls of the uterus. Your doctor may recommend the following for the treatment of [15] uterine polyps. In some cases, the polyps disappear on their own with time.
1. Medication
Drugs that can help regulate the imbalance in hormonal levels can be used as a temporary form of treatment. Medications such as progestins or gonadotropin-releasing hormone agonists [16] can help relieve the symptoms associated with polyps. There is no assurance that the polyps will disappear after taking the medicines, as it will reappear once the medicines are stopped.
2. Surgical removal
If the condition moves to a severe side, your doctor will advise you to get the polyp surgically removed. The surgery will be carried out using a [17] hysteroscope. This can cause mild cramps and slight bleeding and you will be advised to take rest till the surgical incision heals.
Home Remedies For Uterine Polyps
Although there is no definite scientific proof that supports the claim that home remedies can help prevent the onset of the onset of uterine polyps, it is advised that you adopt the following preventive measures.
- Use natural-based feminine care products which will not hinder with your pH levels.
- Avoid simple carbohydrates including sugar, sodas etc.
- Consume foods that are rich in fibre.
- Avoid excessive consumption of caffeine beverages.
Disclaimer: The information provided in this article is for general informational and educational purposes only and is not intended as a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or a qualified healthcare provider with any questions you may have regarding a medical condition.
- [1] DeWaay, D. J., Syrop, C. H., Nygaard, I. E., Davis, W. A., & Van Voorhis, B. J. (2002). Natural history of uterine polyps and leiomyomata.Obstetrics & Gynecology,100(1), 3-7.
- [2] Dreisler, E., Sorensen, S. S., Ibsen, P. H., & Lose, G. (2009). Prevalence of endometrial polyps and abnormal uterine bleeding in a Danish population aged 20–74 years.Ultrasound in Obstetrics and Gynecology,33(1), 102-108.
- [3] Shushan, A., Revel, A., & Rojansky, N. (2004). How often are endometrial polyps malignant?.Gynecologic and obstetric investigation,58(4), 212-215.
- [4] Dreisler, E., Sorensen, S. S., Ibsen, P. H., & Lose, G. (2009). Prevalence of endometrial polyps and abnormal uterine bleeding in a Danish population aged 20–74 years.Ultrasound in Obstetrics and Gynecology,33(1), 102-108.
- [5] De Vaate, A. B., Brölmann, H. A. M., Van der Voet, L. F., Van Der Slikke, J. W., Veersema, S., & Huirne, J. A. F. (2011). Ultrasound evaluation of the Cesarean scar: relation between a niche and postmenstrual spotting.Ultrasound in Obstetrics & Gynecology,37(1), 93-99.
- [6] Albers, J. R., Hull, S. K., & Wesley, R. M. (2004). Abnormal uterine bleeding.American family physician,69(8), 1915-1934.
- [7] Sheth, S., Hamper, U. M., McCollum, M. E., Caskey, C. I., Rosenshein, N. B., & Kurman, R. J. (1995). Endometrial blood flow analysis in postmenopausal women: can it help differentiate benign from malignant causes of endometrial thickening?.Radiology,195(3), 661-665.
- [8] Nalaboff, K. M., Pellerito, J. S., & Ben-Levi, E. (2001). Imaging the endometrium: disease and normal variants.Radiographics,21(6), 1409-1424.
- [9] Anastasiadis, P. G., Koutlaki, N. G., Skaphida, P. G., Galazios, G. C., Tsikouras, P. N., & Liberis, V. A. (2000). Endometrial polyps: prevalence, detection, and malignant potential in women with abnormal uterine bleeding.European journal of gynaecological oncology,21(2), 180-183.
- [10] Jansen, F. W., Vredevoogd, C. B., Van Ulzen, K., Hermans, J. O., Trimbos, J. B., & Trimbos-Kemper, T. C. (2000). Complications of hysteroscopy: a prospective, multicenter study.Obstetrics & Gynecology,96(2), 266-270.
- [11] Pieterse, M. C., Vos, P. L. A. M., Kruip, T. A., Wurth, Y. A., Van Beneden, T. H., Willemse, A. H., & Taverne, M. A. M. (1991). Transvaginal ultrasound guided follicular aspiration of bovine oocytes.Theriogenology,35(4), 857-862.
- [12] Parsons, A. K., & Lense, J. J. (1993). Sonohysterography for endometrial abnormalities: preliminary results.Journal of Clinical Ultrasound,21(2), 87-95.
- [13] Langer, R. D., Pierce, J. J., O'hanlan, K. A., Johnson, S. R., Espeland, M. A., Trabal, J. F., ... & Scully, R. E. (1997). Transvaginal ultrasonography compared with endometrial biopsy for the detection of endometrial disease.New England Journal of Medicine,337(25), 1792-1798.
- [14] Stock, R. J., & Kanbour, A. N. I. S. A. (1975). Prehysterectomy curettage.Obstetrics and Gynecology,45(5), 537-541.
- [15] Tjarks, M., & Van Voorhis, B. J. (2000). Treatment of endometrial polyps.Obstetrics & Gynecology,96(6), 886-889.
- [16] Williams, A. R., Bergeron, C., Barlow, D. H., & Ferenczy, A. (2012). Endometrial morphology after treatment of uterine fibroids with the selective progesterone receptor modulator, ulipristal acetate.International journal of gynecological pathology,31(6), 556-569.
- [17] Sardo, A. D. S., Calagna, G., Guida, M., Perino, A., & Nappi, C. (2015). Hysteroscopy and treatment of uterine polyps.Best Practice & Research Clinical Obstetrics & Gynaecology,29(7), 908-919.



 Click it and Unblock the Notifications
Click it and Unblock the Notifications
