Just In
- 55 min ago

- 2 hrs ago

- 3 hrs ago

- 3 hrs ago

Don't Miss
- Movies
 Bade Miyan Chote Miyan Box Office Day 14: Akshay’s Film Struggles To Touch 60Cr; To Record Its Lowest Number
Bade Miyan Chote Miyan Box Office Day 14: Akshay’s Film Struggles To Touch 60Cr; To Record Its Lowest Number - Sports
 Nitish Rana gets emotional while talking about his handicapped father driving Maruti 800 automatic
Nitish Rana gets emotional while talking about his handicapped father driving Maruti 800 automatic - News
 Dry Days In Kerala: Alcohol Sales Banned For 3 days As Liquor Shops, Bars Remain Closed - Timings & Details
Dry Days In Kerala: Alcohol Sales Banned For 3 days As Liquor Shops, Bars Remain Closed - Timings & Details - Travel
 Mumbai Opens BMC Headquarters For Exclusive Heritage Tour
Mumbai Opens BMC Headquarters For Exclusive Heritage Tour - Automobiles
 The Rise and Fall of the TVS Jive: India's Pioneering Clutchless Motorcycle
The Rise and Fall of the TVS Jive: India's Pioneering Clutchless Motorcycle - Education
 TS Inter Results 2024 Toppers' List, Check Out the Districts That Top the List
TS Inter Results 2024 Toppers' List, Check Out the Districts That Top the List - Finance
 PayU Gets RBI's In-principle Nod To Operate As Payment Aggregator
PayU Gets RBI's In-principle Nod To Operate As Payment Aggregator - Technology
 Realme Narzo 70 5G, Narzo 70x 5G Launched in India: Check Price, Specs, Availability
Realme Narzo 70 5G, Narzo 70x 5G Launched in India: Check Price, Specs, Availability
Bunions: Causes, Symptoms, Diagnosis, Treatment And Prevention
A bony bump that forms on the joint at the base of your big toe is known as a bunion. This condition occurs when your big toe pushes against your next toe making your big toe get bigger and stick out [1] . The skin around the bunion tends to be red and sore. Wearing shoes that are tight and narrow make this condition worse. An inherited structural defect, a medical condition such as arthritis or stress on your foot can be the other reasons why bunions can develop. There can be smaller bunions (bunionettes or tailor's bunion) that can develop on the joint of the little toe [2] . Read on to know more about this condition.
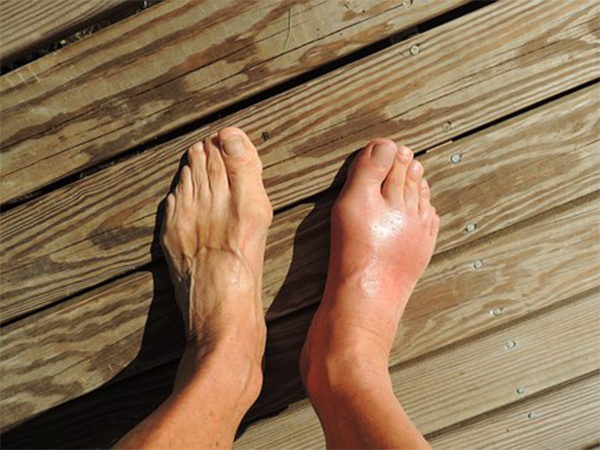
What Is A Bunion?
The point where your big toe meets your foot is known as the metatarsophalangeal (MTP) joint [3] . When a bony bump forms at this joint, it is called a bunion. This condition develops quite slowly, but eventually gets quite bigger and sticks out. It can lead to the big toe turning in. The condition can get quite worse such that sometimes the big toe moves on top of the toe next to it.
The technical term for bunions is hallux valgus[4] . Usually, the symptoms of bunions occur in adults but sometimes adolescents might also experience them. However, in some cases, people might have bunions but without developing any symptoms.
Causes Of Bunions
Few researchers believe that people inherit the bone structure that causes bunions to develop. The following are some of the factors that add to the risk of bunion growth [5] :
•
Foot
injuries
•
Types
of
arthritis,
such
as
rheumatoid
arthritis
•
Overpronation
[6]
(a
low
arch
or
uneven
weight-bearing
in
the
foot
and
tendon
causing
the
toe
joint
to
become
unstable)
•
Hypermobility
[7]
(a
big
toe
bone
that
moves
more
than
required)
•
Polio
and
similar
conditions
(ones
that
affect
both
the
nerves
and
muscles)
The risk of bunion also increases if the feet do not develop properly before birth. Use of high-heeled or narrow shoes can promote the growth of as well as aggravate already-existing bunions.
Use of incorrect footwear does not cause bunions directly but has been seen to be the causative factor behind the development of the defect in people with a genetic risk of the condition. In young people, the bunion will most likely not cause any problem while moving the toe up and down, whereas, in adults, a bunion is more likely to restrict movement.

Symptoms
Of
Bunions
The major symptom is the bump that appears at the base of the big toe. These can also form at the base of the little toe. The other general symptoms of this condition are as follows [8] :
•
A
burning
sensation
•
Pain
and
soreness
•
Numbness
•
Redness
•
Hardened
skin
under
the
foot
•
Swelling
at
the
affected
joint
•
Increased
skin
thickness
at
the
base
of
the
affected
toe
•
Bump
on
the
base
of
the
affected
toe
•
Presence
of
corns
•
Movement
restriction
of
the
affected
toe
The
symptoms
get
worse
when
one
wears
narrow
shoes
and
high
heels
[9]
.Even
standing
for
a
long
time
may
worsen
the
symptoms.
Bunions
start
as
small
lumps.
They
get
worse
over
time
causing
pain
and
making
it
difficult
to
walk.
Complications Related To Bunions
Bunions can lead to the development of the following other conditions [10] :
•
Arthritis
•
Pain
•
Calluses
•
Metatarsalgia
(swelling
and
pain
in
the
ball
of
the
foot)
[11]
•
Difficulty
walking
•
Decreased
mobility
in
the
toes
•
Bursitis
(Swelling
in
the
fluid-filled
pads
that
cushion
the
bones,
muscles
and
tendons)
[12]
•
Hammertoe
(abnormal
joint
bending)
[13]

To prevent these complications from occurring, avoid shoes that cramp the feet in one way. Your shoes should conform to the shape of your feet (without any squeezing or pressing on any part of the foot). Opt for shoes that have a wide toe box (no pointy toes).
Try to find a good-fitting shoe where there is comfortable spacing between the tip of your longest toe and the end of the shoe.
Diagnosis Of Bunions
Examination of the foot is the most ideal way a doctor identifies the presence of a bunion. Further, an x-ray of your feet can also help the doctor identify the cause of the bunion and analyze its severity so that the next stage of treatment can be understood [14] .
Treatment For Bunions
Medications and surgery are the two main options available to treat bunions.
•
Medications:
These
can
help
with
pain
and
swelling
[15]
.
◦
Pain-relieving
medications:
Over-the-counter
pain
relieving
medicines
can
reduce
the
pain
and
swelling
to
a
great
extent.
◦
Cortisone
injections
[16]
:
These
are
used
to
get
rid
of
the
swelling.
These
are
ideally
focused
on
the
fluid-filled
pads
that
cushion
the
bones.
[bunion
injection
image]
•
Surgery:
Some
people
suffering
from
bunions
might
need
surgical
intervention.
Surgery
is
opted
for
the
following
people
[17]
:
◦
Those
who
cannot
bend
or
straighten
a
toe
(usually
due
to
stiffness)
◦
Those
who
have
a
deformity
that
is
quite
severe
(toe
crossing
over
another
toe)
◦
Those
who
experience
pain
and
inflammation
that
does
not
reduce
with
other
treatments
The surgical intervention aims at relieving pain, realignment of the metatarsophalangeal joint and correction of other deformities causing the problem. The treatment of bunions might include the following surgical procedures:
•
Repair
of
the
tendons
and
ligaments:
This
involves
lengthening
the
toe
and
shortening
any
weak
joint
tissue.
•
Osteotomy:
This
is
used
to
realign
the
joint
[18]
.
Pins,
screws
and
plates
are
used
to
fix
the
bone.
•
Arthrodesis:
This
involves
the
removal
of
the
swollen
joint
surface
[19]
.
To
hold
the
joint
together
during
healing
wires,
screws
or
plates
are
used.
•
Exostectomy:
The
bump
on
the
toe
joint
is
removed
[20]
.
This
form
of
surgical
intervention
does
not
treat
the
underlying
cause
of
the
bunion.
•
Resection
arthroplasty:
This
removes
the
damaged
portion
of
the
toe
joint[21]
This
procedure
is
usually
performed
on
older
adults
with
a
bunion
or
on
those
who
have
severe
arthritis.
Lifestyle Tips To Deal With Bunions

•
Applying
ice
to
the
affected
area
can
reduce
swelling.
•
Orthotic
shoe
inserts
can
relieve
pressure
on
the
toe.
•
Padding,
taping
or
splinting
of
the
toe
can
provide
support
and
reduce
irritation.
•
Avoid
activities
that
can
increase
pain
such
as
playing
contact
sports
or
standing
for
a
long
period
of
time.
- [1] Ferrari J. (2009). Bunions.BMJ clinical evidence,2009, 1112.
- [2] Ajis, A., Koti, M., & Maffulli, N. (2005). Tailor’s bunion: a review.The Journal of foot and ankle surgery,44(3), 236-245.
- [3] Chou, L. B. (2000). Disorders of the first metatarsophalangeal joint: Diagnosis of great-toe pain.The physician and sportsmedicine,28(7), 32-45.
- [4] Wülker, N., & Mittag, F. (2012). The treatment of hallux valgus.Deutsches Arzteblatt international,109(49), 857–868.
- [5] Nguyen, U. S., Hillstrom, H. J., Li, W., Dufour, A. B., Kiel, D. P., Procter-Gray, E., … Hannan, M. T. (2010). Factors associated with hallux valgus in a population-based study of older women and men: the MOBILIZE Boston Study.Osteoarthritis and cartilage,18(1), 41–46.
- [6] Wallden, M. (2015). Don't get caught flat footed–How over-pronation may just be a dysfunctional model.Journal of bodywork and movement therapies,19(2), 357-361.
- [7] Doty, J. F., & Coughlin, M. J. (2013). Hallux valgus and hypermobility of the first ray: facts and fiction.International orthopaedics,37(9), 1655–1660.
- [8] Fraissler, L., Konrads, C., Hoberg, M., Rudert, M., & Walcher, M. (2016). Treatment of hallux valgus deformity.EFORT open reviews,1(8), 295–302.
- [9] Robinson, C., Bhosale, A., & Pillai, A. (2016). Footwear modification following hallux valgus surgery: The all-or-none phenomenon.World journal of methodology,6(2), 171–180.
- [10] Ferrari J. (2014). Hallux valgus (bunions).BMJ Clinical Evidence,2014, 1112.
- [11] Mulder, J. D. (1951). The causative mechanism in Morton's metatarsalgia.The Journal of bone and joint surgery. British volume,33(1), 94-95.
- [12] Blackwell, J. R., Hay, B. A., Bolt, A. M., & Hay, S. M. (2014). Olecranon bursitis: a systematic overview.Shoulder & elbow,6(3), 182-190.
- [13] Higgs S. L. (1931). Hammer Toe.Postgraduate medical journal,6(68), 130–132.
- [14] Pourhoseingholi, E., Pourhoseingholi, M. A., Bagheri, A., Esfandiar, E., & Saeb, M. (2017). Footprint as an alternative to X-ray in hallux valgus angle measurement.Medical journal of the Islamic Republic of Iran,31, 33.
- [15] Tamer, P., & Simpson, S. (2017). Evolutionarily medicine Why do humans get bunions?.Evolution, medicine, and public health,2017(1), 48–49.
- [16] Grice, J., Marsland, D., Smith, G., & Calder, J. (2017). Efficacy of foot and ankle corticosteroid injections.Foot & ankle international,38(1), 8-13.
- [17] Scranton Jr, P. E. (1983). Principles in bunion surgery.JBJS,65(7), 1026-1028.
- [18] Lee, D. C., & Byun, S. J. (2012). High tibial osteotomy.Knee surgery & related research,24(2), 61–69.
- [19] Yasui, Y., Hannon, C. P., Seow, D., & Kennedy, J. G. (2016). Ankle arthrodesis: A systematic approach and review of the literature.World journal of orthopedics,7(11), 700–708.
- [20] McBeth, Z. L., Galvin, J. W., & Robbins, J. (2018). Proximal to Distal Exostectomy for the Treatment of Insertional Achilles Tendinopathy.Foot & ankle specialist,11(4), 362-364.
- [21] Rüther, W., Verhestraeten, B., Fink, B., & Tillmann, K. (1995). Resection arthroplasty of the metacarpophalangeal joints in rheumatoid arthritis: results after more than 15 years.Journal of Hand Surgery,20(5), 707-715.
-
 healthHow To Keep Feet Hot During Winters: 12 Tips That Will Tackle Cold Feet Issues And Make Your Feet Thank You
healthHow To Keep Feet Hot During Winters: 12 Tips That Will Tackle Cold Feet Issues And Make Your Feet Thank You -
 health5 Reasons Why Your Feet Become Numb Quick
health5 Reasons Why Your Feet Become Numb Quick -
 beautyFoot Packs To Get Rid Of Dry Foot Skin
beautyFoot Packs To Get Rid Of Dry Foot Skin -
 wellness6 Common Warning Signs Your Feet Can Show About Your Health
wellness6 Common Warning Signs Your Feet Can Show About Your Health -
 wellnessDid You Know These Benefits Of Massaging Feet Before Bedtime?
wellnessDid You Know These Benefits Of Massaging Feet Before Bedtime? -
 wellnessWhat Your Feet Say About Your Health: Know About The 15 Warning Signs And Ways To Keep Your Feet Healthy
wellnessWhat Your Feet Say About Your Health: Know About The 15 Warning Signs And Ways To Keep Your Feet Healthy -
 diabetes12 Safe And Effective Tips For Diabetic Foot Care
diabetes12 Safe And Effective Tips For Diabetic Foot Care -
 body careHow To Use Pumice Stone To Heal Dry And Cracked Feet
body careHow To Use Pumice Stone To Heal Dry And Cracked Feet -
 disorders cureWhat Are Corns And Calluses? Causes, Symptoms, Risk Factors, Treatments And Prevention
disorders cureWhat Are Corns And Calluses? Causes, Symptoms, Risk Factors, Treatments And Prevention -
 body care8 Wonderful Tips To Take Care Of Your Feet This Winter Season
body care8 Wonderful Tips To Take Care Of Your Feet This Winter Season -
 skin careUse These Amazing Essential Oil Remedies To Treat Dry Feet
skin careUse These Amazing Essential Oil Remedies To Treat Dry Feet -
 body careTry These Home-made Foot Scrubs To Get Beautiful & Soft Feet
body careTry These Home-made Foot Scrubs To Get Beautiful & Soft Feet


 Click it and Unblock the Notifications
Click it and Unblock the Notifications



